Limb pins and needles, numbness during cycling - physiotherapeutic clinical reasoning
by Martin Krause
Introduction of examination and assessment process
Cyclists frequently complain of pins & needles and numbness in their feet. The physiotherapist can ascertain the origin of this problem through a process of elimination whereby a structured and systematic examination process leads to a specific diagnosis and hence management strategy.
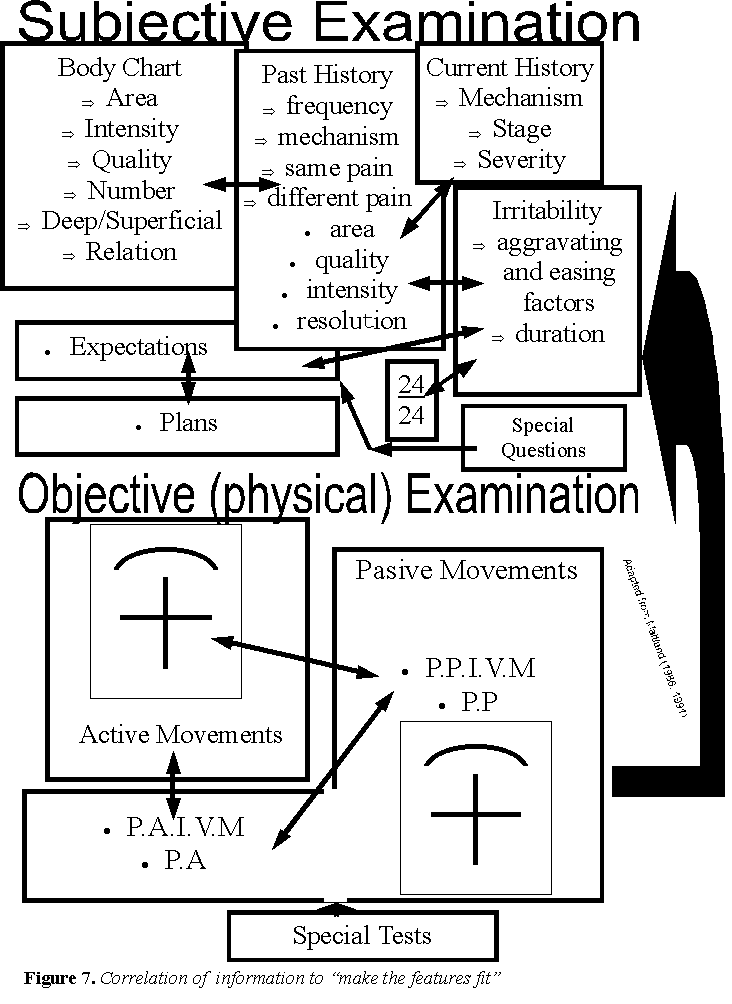
Musculoskeletal pathology in the spine can contribute to altered sensations in the limbs
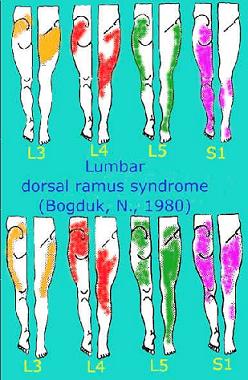
Similar altered sensations can occur in the upper limb. It doesn't have to be from spinal pathology. Other causes can be mechanical irritation in periphery, affecting neural and/or vascular tissue. Differential diagnosis becomes an important strategy in the treatment of limb pins and needles, numbness and altered sensations when cycling.
The clinical reasoning process
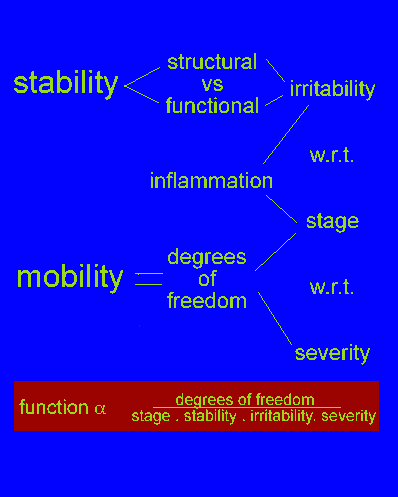
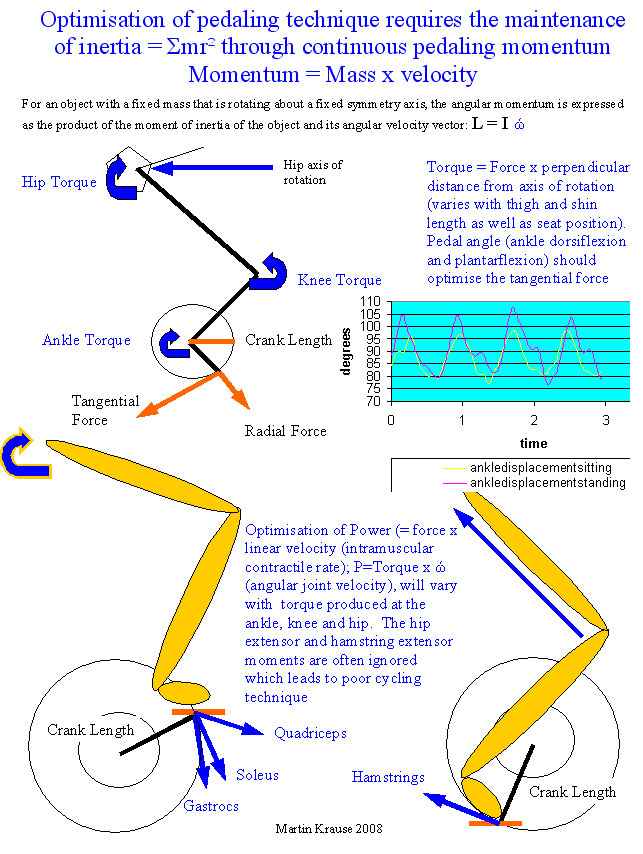
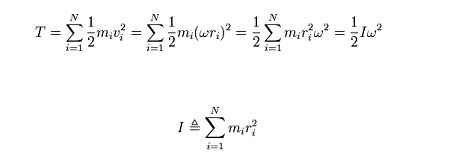
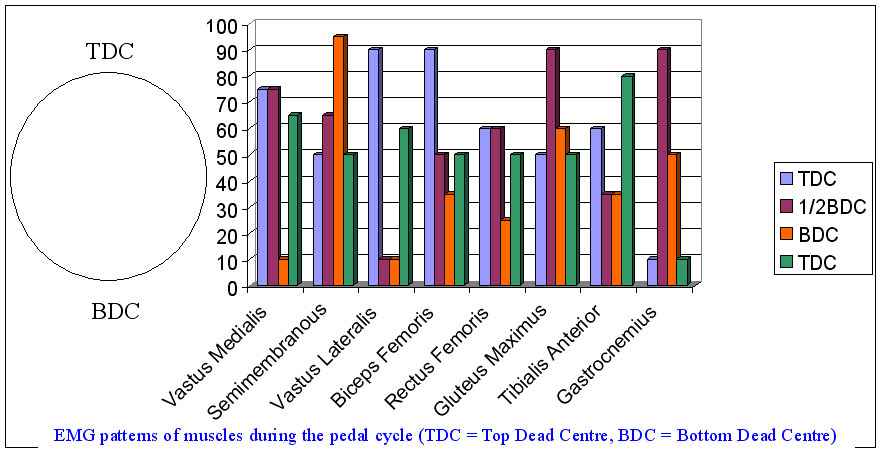
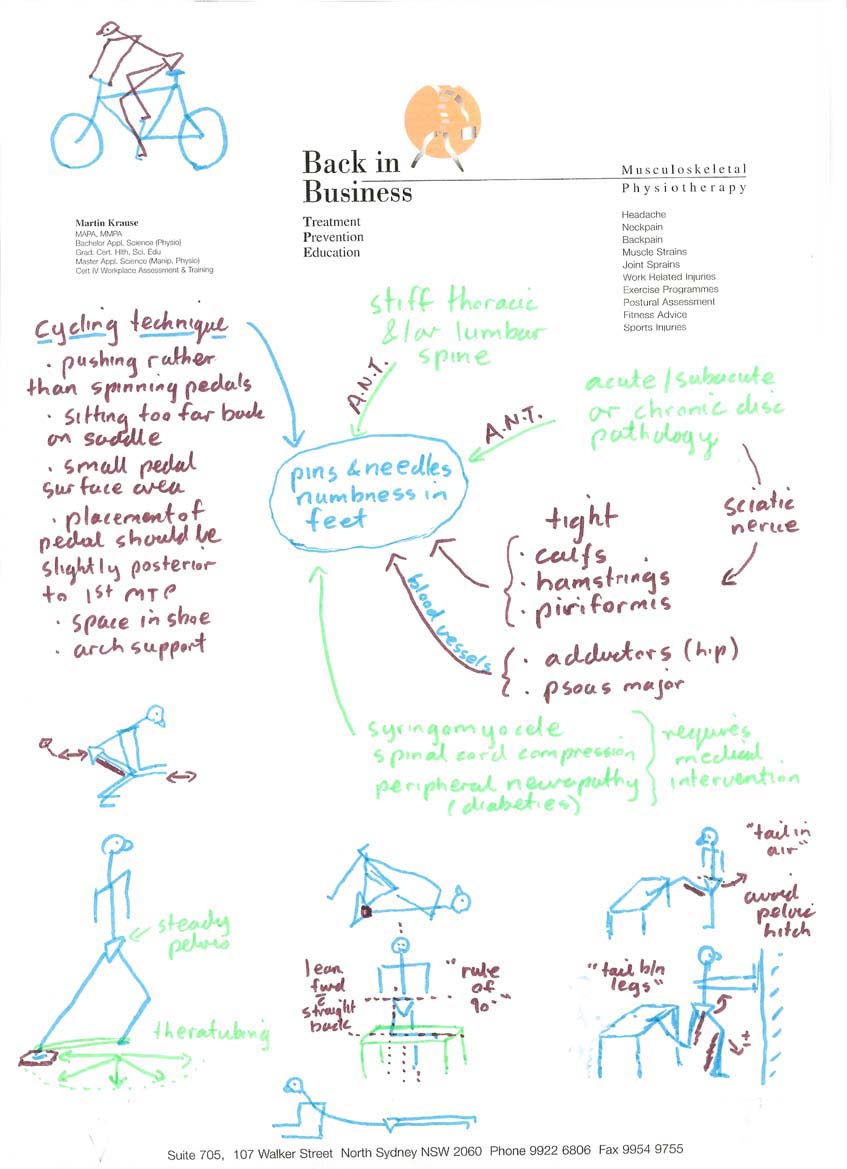
The following represents a 'mind-map' of various possibilities which can cause the feet 'to go to sleep', as well as outlining some common stretches which cyclists can undertake to try to ameliorate the condition.
Mind Map
ANT = adverse neural tension
Adverse Neural Tension
Since the blood vessels frequently course in parallel through potentially compromising anatomical structures, virtual canals between bones, muscles and ligaments, tension in muscles or irritation from soft tissue structures, such as myofascia, disc and ligaments, can lead to direct mechanical compromise of blood vessels as well as the blood vessels of the nerves themselves. Commonly referred to Adverse Neural Tension (ANT). Piriformis syndrome in the butt is a common example. Another complication of cycling can be direct compression of the pudendal nerve from an incorrect saddle as seen here : https://back-in-business-physiotherapy.com/we-treat/pelvic-floor-pain.html. The obturator internus muscle has fascia which is continuous with the pelvic floor. Both the obturator internus and externus are external rotators of the hip. Trigger points in any of the muscles around the pelvis and upper leg can lead to pain and/or strange sensations of numbness causing all the way down the leg. Read more : https://www.back-in-business-physiotherapy.com/we-do/trigger-point-massage.html
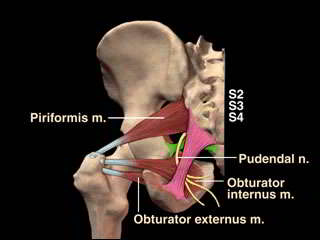
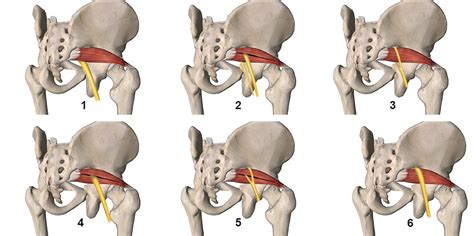
Piriformis Syndrome
This is probably the most common form of adverse neural tension, whereby a tight piriformis leads to compression of the sciatic nerve. Anatomically, the sciatic nerve lies underneath the piriformis. In about 10% of the population, it actually run through the substance of the muscle itself, have bifurcations as well as run over the top of the muscle..
Paraesthesia hyperaesthetica (meralgia) lateral femoral cutaneous nerve
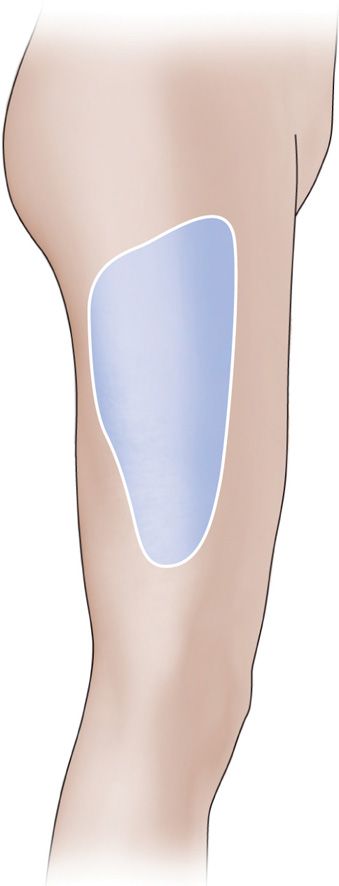
Another form of ANT resulting in lateral thigh numbness and/or pain is from compromise of the lateral femoral cutaneous nerve in the superior groin region.
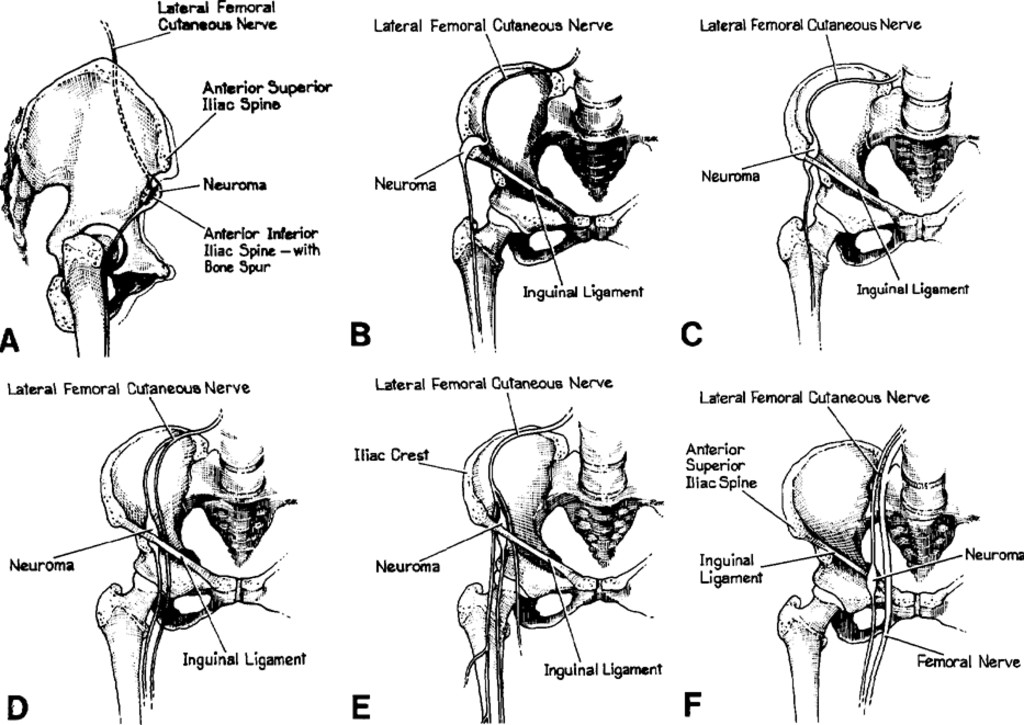
Mind map for multiple hypothesis formation (vascular conditions are considered separately below)
The Bike
The positioning on the bike is critical to comfort, power and optimal efficiency. Many myths exist as to what is the ideal position. Quite simply, the best position is the one that sounds best. When a person is positioned correctly on the bike, the pedalling action will sound very efficient - smooth spinning rather than stroking.
The frame : for women this can be a big issue. Smaller frames tend to have much steeper downtube angles making adjustments more critical. In my experience, bigger people tend to be on frames too big for them. Generally speaking, a frame that is too large results in the cyclist over-reaching and/or floating sideways over the bike. A frame which is too small results in anterior knee pain. However, smaller frames can have their seat height adjusted.
Are they in the correct position?
- Ideally, the cyclist should be able to place their hands comfortably on all 3 positions of the handle bars. Once they are in those positions, they should be able to easily lift their hands slightly off the handle bars. This is called the "centre of balance approach". If they cannot do this, then either they have reduced core strength or their seat is in the incorrect position or both. Remember when moving the seat forward, it rises on the rail and vice versa on the way back. The longer the torso the further back the seat can go. Importantly, the lung capacity should be reduced due to an over-arched back. Since 20 muscles are involved with breathing and 18 of these are postural muscles (Steve Hogg), these postural muscles need to be activated as minimally as possible without compromising stability. Additionally, if the cyclist is a toe dipper they tend to pull the body forward and hence the seat should be further back. Conversely, the heel dropper should have the seat further forward. Regardless, the seat positioning should make the arm load insignificant, thereby allowing those muscles to be used for comfortable and effective breathing. Hereby, energy and blood flow isn't wasted by going to muscles which are working 'over-time'.
There are three areas where bike adjustments are looked at
- the saddle - the less padding the better, wider and flatter seats for females, wear on the seat should be from the sitting bones. Seats which are too high result in posterior knee pain, seats which are too low result in anterior knee pain and sometimes groin pain, seats which are too far back and/or too high can result in lateral knee pain and even cause deep peroneal nerve injury. Ideally, the seat is just behind 'bottom centre'.
- the pedal - a free floating pedals (free play cleat) tend to take away the need for critical adjustments. Generally the foot should be as far forward as the cleats allow. This latter aspect will depend on shoe size. By reducing the distance from the pedal to the ankle, it is thought that the need to stabilize the foot is reduced thereby allowing the muscles to concentrate their force for developing power.
- the handlebars and stem - the bend is critical as there should be enough space on the drops for bigger hands, and conversely smaller hands need the ability to correctly position brake levers for smaller fingers to reach the brakes when on the drops. Handlebars which are too low tend to place a lot of pressure on the genital area. Symptoms of too much perotineal pressure include rounding the back and keeping the pelvis upright. Stems which are too short or too long can overload the upper torso, arm and neck musculature.
The Foot
Forefoot varus - over pronation of forefoot can induce small surface area loading resulting in pain, pins & needles and numbness. A Mortons Neuroma may also be an issue. Lemond LeWedges and other wedges can be inserted onto the medial side of your pedals which not only should take away the symptoms in the foot, they should also be able to help any medial knee pain as well. Furthermore, with a more even distribution of force across the forefoot, the pedalling efficiency should improve.




These can also be used to correct leg length discrepancies. It should be noted that we don't directly endorse these products but have used them here for descriptive clarification purposes only. Many 'bike fit' specialists design and fit their own custom-made wedges, spacers and insoles.
Insoles with various height arch supports and/or internal wedging can also be used to aid in the development of power and torque across the foot as well as reduce the effect of arch elongation on neurovascular dynamics which may be leading to pins & needles and numbness in the feet.
The Pelvis
Do they have an Anterior Pelvis X'ed Syndrome (APXS) - posterior pelvic tilt (butt clencher) or do they have a Posterior Pelvis X'ed Syndrome (PPXS) - anterior pelvic tilt? Extremes of pelvic tilt can also lead to reduced gluteal - abdominal muscle synergies.
Assess the pelvis for static and dynamic asymmetry
How do the internal stabilizing 'guy wires' act to support the external 'slings'?
The Slings

The Diaphragm
Assess the diaphragm for lateral movement, iliopsoas function and costothoracic spine mobility as this can potentially affect the pressure on both the aorta and it's branches as well as the vena cava and it's branches
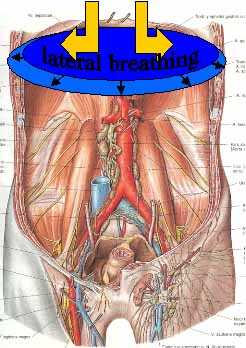
The tension in the Psoas Major can be palpated by the physiotherapist through an anteriomedial direction, just lateral to the rectus abdominis with the client in supine. Enhanced tension and symptoms are usually quite obvious when present. Then, the next important factor is to ascertain whether the muscle changes it's relaxed tension during lateral breathing. Pressure relaxation techniques and lateral breathing are quite useful to restore the normal spectrum of Psoas Major contraction-relaxation cycle. The therapist should reassess the inguinal pulse for improved circulation. Then the Psoas Major should be assessed in side lying during isometric hip flexion on both the ipsilateral and contralateral sides. Quite frequently, contralateral isometric hip flexion results in excessive muscle contraction due to Newtons Third Law of action-reaction. The client can be taught to ascertain the tension in Psoas Major through palpation in side lying and/or relaxed sitting with isometric hip flexion, using the lateral breathing technique. Once they have mastered the activity in the safety of their home or office environment, then it could also be practiced on the bike.
Interestingly, some of the yoga positions such as the sun salutations with Knee flexion can exert considerable tension on the Psoas Major and the abdominal aorta resulting in foot numbness
Although, the above yoga positions are good for some people, many are impossible for the average person or for a person with spinal or other joint pathology, This is where professional advice comes into play. The following exercise, frequently reproduces feet numbness in my clients. In some instances, it's purely associated with tight hip flexors and quadriceps, or peripheral sympathetic nervous system ganglia stimulations, whereas, in other people it may be associated with spinal canal narrowing.
Hip and back exercises
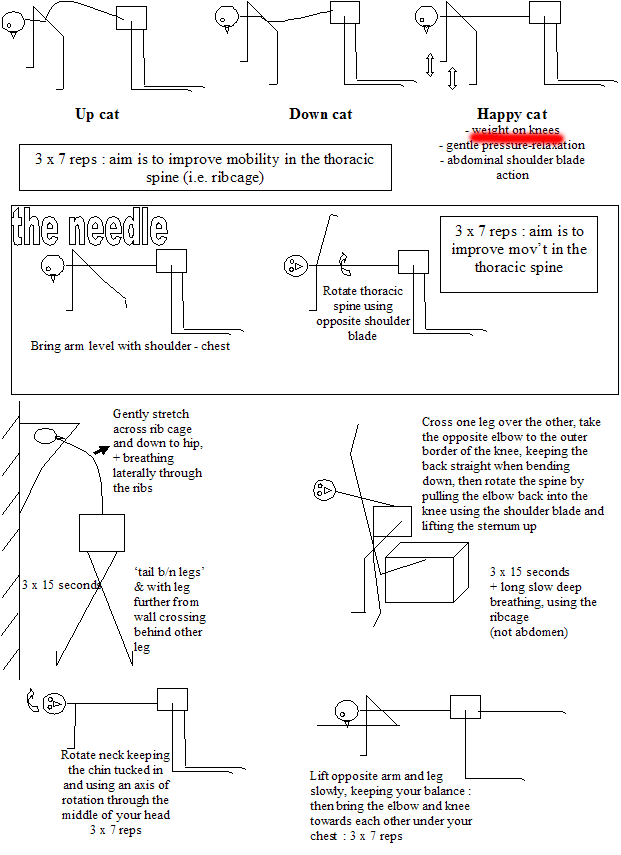
Some stretches, strengthening, stabilisation and co-ordination for the thoracic spine and lower limbs
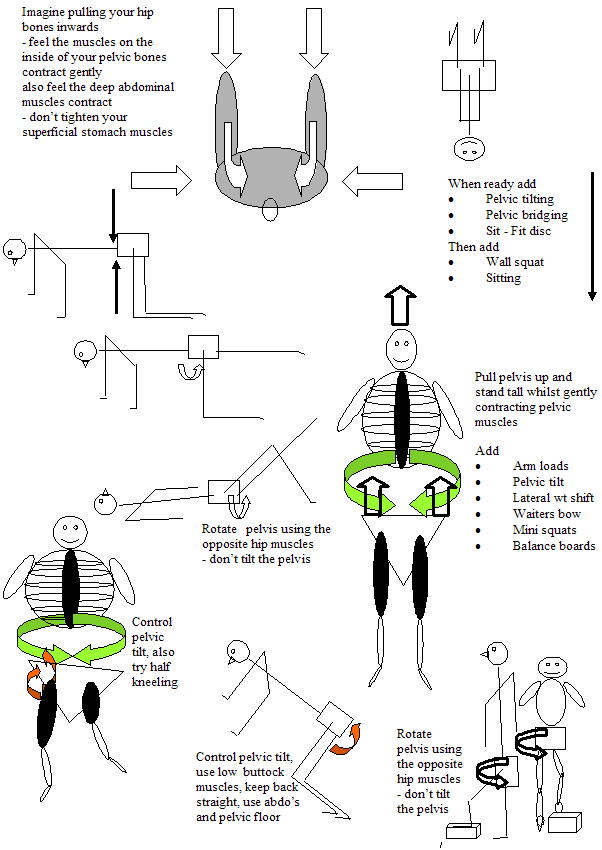
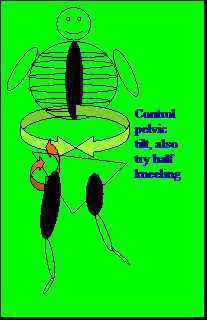
Hip pelvic control and mobility
Asymmetry of leg power
A frequent clinical observation are not only the structural asymmetries of static and dynamic posture, but also variation in muscle bulk and power. Perhaps due to the nature of cycling it may be possible to compensate for asymmeterical strength through pedalling cadence. However, as the demands of cycling are increased, either through higher power output or longer duration, then loading intolerance due to pedalling inefficiency becomes critical.
It is recommended that the cyclist should be assessed whilst being loaded on their bike. In this way the correct set-up can be ascertained as well as imbalances in power output deduced. The client should be given strategies to emphasise the weaker leg, such as commencing and emphasising the pedalling stroke on the weaker side. Essentially, for endurance this is best done going uphill at 60 RPM, for power a much lower cadence (even 30RPM) is recommended where resistance is the critical factor. Importantly, this latter exercise should only be undertaken for short periods (10-20 minutes) and repeated only after 72hours of recovery and not in the competition season. Naturally, the person should stay seated.
Other forms of developing power is to emphasise exercises for the quadriceps and gluteal muscles. These include 1 leg squats whereby external stabilising mechanisms such as hand holds or butt against the wall can be used to maintain good form. The squat probably doesn't need to be deeper than 120 degrees knee bending. To obtain gluteal contraction, it is necessary to bend forward in the hips (to b/n 80-100 degrees) whilst keeping the back straight. Initially, commence with 3 sets of 7 reps with a few minutes rest b/n sets for recovery, later sessions should eventually build up to 5 sets of 15 reps with 30-120 secs break b/n sets depending upon the perceived intensity and rate of recovery.
Core stability training using the Swiss ball in side lying can be very advantageous to build the power and agility b/n the hip and back. This involves lying on the side with the ball b/n the feet. The legs and pelvis are in line with the body. The pelvis should NOT MOVE. Initially, commence by rotating the ball around the bottom leg. If superficial leg muscles are used for this (e.g ITB/TFL) then the pelvis will move. If however, the deep hip rotators, pelvic floor and deep abdominals are used then the pelvis will remain steady. additionally, some nice synergistic action with the back erector spinae will also occur. 3 x 30 reps
Next, try to make the same movement of the ball around the stabilised but lifted off the bed lower leg. In this case superficial abdominal and hip muscles are used to produce power and stability through agility. This latter exercise does NOT replace the previous one just because it is harder. Both exercises look similar but are activating different muscles due to varying loading thresholds. Endurance muscles are slow twitch low loading exercises, whilst the sprint muscles are high load, fast twitch muscles. 3x 7 reps building up to 5 x 15 reps
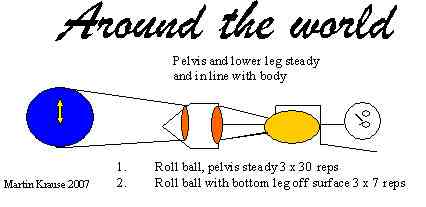
If there is some doubt to the presence of an abdominal aneurysm or aortic stenosis then pulses and blood pressure should be tested during this exercise and the abdominal pulse should be auscultated using a stethoscope (see below). Naturally, this exercise should be ceased immediately if there is the slightest doubt to the presence of vascular insufficiency.
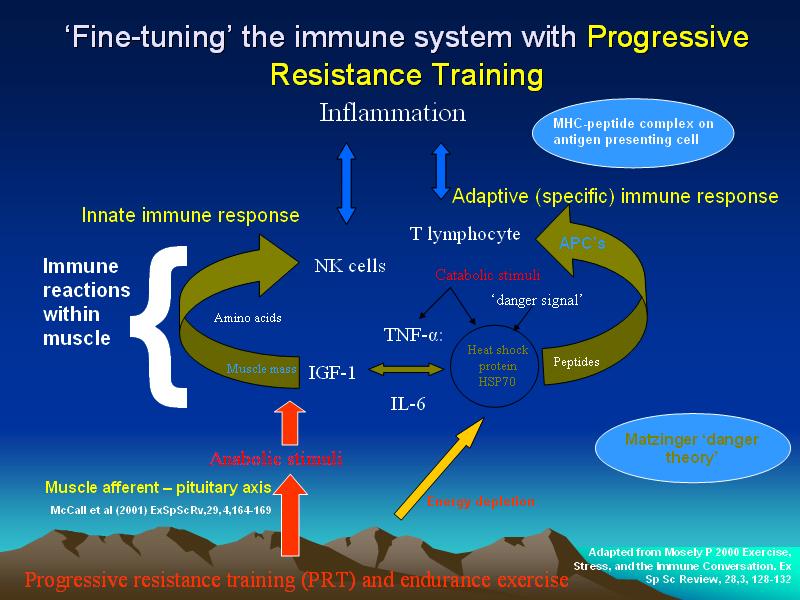
Immune System
Immune system issues can also exaggerate pedalling asymmetries. If the body has used muscle protein for fighting off infection or disease then muscles which already are weak, appear even weaker. This weakness may result in excessive stiffness and/or fatigue. With fatigue form break down and with stiffness joints and tendons are excessively loaded. Depending upon the severity of the illness I suggest giving your body up to 6 weeks to recover through graded and gradual return to training.
see : Link to Immune System and Training and Link to Endurance Training (Periodisation) and Link to Nutrition for recommendations on recovery after illness or injury.
Cross Training
Having worked with Tour de France cyclists I understand that cross training may have also created the symptoms. Common forms of cross training which could place excessive pressure on the ball of the foot include
- rowing
- cross-country running
- boxing
Besides stretching, metabolic considerations may include supplementation with fish oil, magnesium, tonic water and vitamin E. A sports nutritionist should be consulted, especially if there is a diabetes component to the problem.
Vascular System
Finally, a less common form of pins & needles in the feet during cycling may be due to claudication. Such claudication may be the result of damage to vessels of the abdominal aortic. Additionally the branches of the abdominal aorta descending into the leg as well as the leg vasculature may be damaged by trauma and/or systemic complications (e.g. Marfan's syndrome, vascular diseases, etc). These problems may be a medical emergency whereby immediate consultation with a vascular surgeon is imperative.
Virchow's Triad in the aetiology of thrombosis may also be of assistance with differential diagnosis. The 3 variables include
- Changes in vessel wall (endothelial damage)
- Changes in blood flow (flow volume/stasis)
- Changes in blood constituents (state of coagulability)
The latter may include screening questions for blood disorders (thrombolytic ones, C-reactive protein , Leiden Factor V, as well as Thalasaemia and Sickle Cell Anaemia), systemic inflammatory conditions (such as Lupus and Scleroderma), the use of oral contraceptives, smoking, diet and frequent flying.
Taylor & Kerry (2005) quote a paper from Sise et al (1989) reporting an average 2 year delay in diagnosis in young people where 93% could have been diagnosed with simple palpation of peripheral pulses.
Vascular complications are potentially overlooked causes of symptoms. This in part may be due to their relative infrequency compared with other conditions seen by physiotherapists. Furthermore, the symptoms of vascular compromise may mimic those of symptoms arising from musculoskeletal structures. Compromise of a blood vessel to the spinal nerve results in radicular pain. A colleague reported the incidental finding of a family friend's teenage boy whose mother was about to take him to the chiropractor for low back pain. What he noted was the boy had 3 socks on his left foot!!! Immediate examination of the lack of pedal pulses and referral to the A+E department confirmed a diagnosis of spinal artery thrombosis. Unfortunately, most peoples friends aren't astute clinicians that recognise "something which doesn't make sense". Arterial kinking of the external iliac artery during hip flexion whilst cycling (and rowing, skating and Fjell running) have been known to produce pain affecting the buttock, anterolateral thigh, calf and foot with feelings of paraesthesia and numbness in the toes. Cyclists may also describe the feeling of 'fullness' in the leg and lack of power, cramping and/or ischaemic like fatigue. Although anterior/posterior and lateral compartment syndromes are commonly associated with vascular complications in running, similar type (not necessarily area) of symptoms associated with iliac artery, femoral artery and popliteal artery can be missed during the clinical reasoning process. Generally, symptoms are associated with exertion and external compromise of the blood vessel. Apart from the iliac artery already mentioned other examples include the femoral artery in the adductor canal (b/n the adductor magnus and vastus medialis), and the popliteal artery interfacing with the medial head of gastrocnemius. Generally, these conditions are associated with anatomical anomalies whereby the external pressure from repetitive movement gradually damages the external lining of the blood vessel. Besides repetitive microtrauma, any external trauma from an accident needs to consider possible vascular damage or the formation of scar tissue and adhesions which could lead to vascular damage. Other clinical examples, include aortic aneurysm which may be due to valsalva type maneuver. Familial history may also be important in differential diagnosis. Additionally, a history of heavy smoking can lead to internal blood vessel pathology. Similarly, women who take the pill may also be at risk. Aortic stenosis may manifest as a result of arterosclerosis or due to underlying congenital defects. These are screening questions which need to be asked during the subjective examination. During the physical examination, the femoral and pedal pulses should be examined at rest but usually need to be assessed immediately after exercise or in the compromising posture where symptoms normally manifest. Further testing should include ankle blood pressure monitoring of each side. Taylor & Kerry (2005) recommend 20 minutes of rest before testing systolic blood pressure in the left and right brachial artery, posterior tibial and dorsalis pedis and then using the "Ankle to brachial pressure index = Ankle systolic BP / Brachial systolic BP". 1 - 1.2 considered normal, 0.75 - 0.9 indicates moderate disease, 0.5 - 0.75 severe disease and <0.5 is limb threatening. (see: Taylor AJ, Kerry R (2005) Vascular syndromes presenting as pain of spinal origin. Ch 36 in Grieve's Modern Manual Therapy: The Vertebral Column. Ed Boyling JD & Jull GA Elsevier Churchill Livingstone).
Compartment syndrome
Compartment syndrome classically refers to the calf muscles, whereby the exercising muscles increase their volume by up to 60% through additional blood flow. The muscles in the calf are surrounded by myofascia, as well as bone. If the myofascia is pliable, the increased size of the calf muscles is accommodated. However, if their pliability is insufficient, arterial pressure allows blood to enter the compartment (100-220mgHg internal pressure), but the venous system is compressed, because the internal pressure (5-15mmHg) is less than the external pressure exerted by the compartment, preventing outflow of blood. In athletes, this will manifest as deep burning pain and potential numbness. In extreme cases, muscle necrosis can occur, which is life threatening. Some athletes have the sickle cell anaemia trait, which makes the blood 'stickier', thereby compromising blood flow even further https://www.back-in-business-physiotherapy.com/latest-news/241-sickle-cell-trait-and-acute-low-back-pain.html. It should be noted that compartment syndrome can occur anywhere in the body that is enveloped and the compromise can come from impact trauma forming haematomas and/or blood clots. In many instances, if misdiagnosed, lack of immediate medical and/or surgical treatment, can be catastrophic.
The Upper Limb and vascular compromise
The posture of the cyclist (and rower) may also make these athletes particularly prone to upper limb and head/neck vascular conditions. Additionally, one of the most common cycling injuries involves landing on the shoulder or outstretched hand resulting in possible neurovascular traction injury, direct trauma and/or clavicular fracture. The latter has been associated with trapezius muscle dysfunction which can be a precipitating variable leading to Thoracic Outlet Syndrome (TOS). Symptoms of TOS can include typical symptoms of neck, shoulder, elbow and hand pain. Occasionally, people describe a sense of swelling (or fullness) in the arm, with/without concommitant pins & needles or numbness. Vascular components of TOS may be less prevalent than neurological ones. Yet this may be due to mis-diagnosis as the plethora of tests (Adson's, Allen's Halstead's maneuver, Roos's EAST test) may be falsely positive or negative and variable b/n examiners. Hence, the examination must use the multitude of variables at the clinicians disposal, both Subjective symptoms & Physical signs - inductive and deductive reasoning, to make sense of the clinical picture. When in doubt and further investigations are required, by using the weight of probability from many variables, it may also make the argument for further testing more convincing to a medical colleague.
Paget - Schroetter syndrome is a deep venous thrombosis of the subclavian - axillary venous system, also known as "effort thrombosis" (Rutherford 1998, Zell et al 2001) and may account for about 3-7% of all DVT's (Taylor & Kerry 2005). The average patient is in their late 20's to early 30's and males present 3 times more commonly than females. Most commonly complain of quick insidious arm pain (70% in dominant arm), with possible supraclavicular fossa and ipsilateral neck pain. Most commonly occurs in activity with repetitive upper arm, over shoulder height, movements. The usual aetiology is Virchow's Triad which means that specific screening questioning is required. Additionally, other risk factors may include thoracic outlet factors such as cervical rib, anomalous first rib, hypertrophy of the anterior scalene, subclavius or pectoralis minor as well as endogenous factors such as activated protein C resistance and anticardiolipin antibodies (Ellis 2000 in Taylor & Kerry 2005).
Taylor & Kerry suggest that observable signs of vascular compromise may include skin pallor or cyanosis - both resting and positional, swelling, and/or superficial venous dilation. Corneal arcus or xanthelasmas (yellowish raises skin changes) around both eyes may be associated with hyperlipidaemia and hypercholesterolaemia. Staining of fingers may be a more accurate indicator of tobacco consumption. Obesity and state of mental awareness may also reflect underlying cerebrovascular state.
Hand and digital examination should also include nail squeezing - indicative of capillary refilling time. These should be performed in various positions of potential vascular compromise. Nail abnormalities may be present. Pulses should be tested, stethoscope auscultation should be undertaken and the pressure cuff sphygmomanometer and hand held doppler or automatic blood pressure monitor used (Taylor & Kerry 2005).
Taylor & Kerry (2005) argue quite strongly that vascular examination is such a miniscule part of both under-graduate and post-graduate degrees that we may be implicated in delayed diagnosis and initiating inappropriate treatment.
An unusual case of Femoral Artery compression can be found here : https://back-in-business-physiotherapy.com/latest-news/274-an-unusual-case-femoral-artery-compression.html
Neuropraxia of median and ulnar nerves
The ulnar nerve is at risk of entrapment in Gyon's Canal around the Hook of Hamate over the Triquetrium (Medial hand). This can lead to pins & needles in the 5th and half of the 4th fingers (little and ring finger). Additionally a loss of pincer grip strength can occur due to the ulnar nerves innervation of the adductor pollicis (webspace b/n index finger and thumb).
The median nerve can become entrapped in the carpal tunnel leading to pins & needles on the palmar surface of the hand and thumb to 4th fingers.
A good pair of gloves as well as appropriate bike set-up (ability to sit on bike with minimal pressure on hands) are usually necessary. Sometimes the brake positioning must also be altered in order to maintain a neutral position of the wrist.
Neck and Thoracic Spine pathology
Dysfunction of the neck and thoracic spine can lead to distal limb symptoms. Additionally, posterior rotator cuff pathology can create radial nerve and lateral elbow symptoms. Displaced clavicular (collar bone) fractures (>2cm) can lead to significant scapula (shoulder blade) mal-positioning giving rise to neck and arms symptoms. Scapula stabilising exercises as well as neck mobility/stability/synergy exercises and physiotherapy can alleviate all these symptoms. Correct bike set-up is also essential.
Read more on vascular compromise : https://back-in-business-physiotherapy.com/latest-news/342-vascular-system-and-musculoskeletal-physiotherapy.html
Cysts
In 2005, I saw 2 clients with Tarlov's cysts in the lumbar spine, thoracic and sacral regions, who presented with some low back pain but predominantly claudication type symptoms (generalised leg symptoms including 'ants crawling' & 'spider crawling') as well as some abdominal bloating. I had seen each of them some time previously for an episode of low back pain. Both had successful surgical intervention.
see also
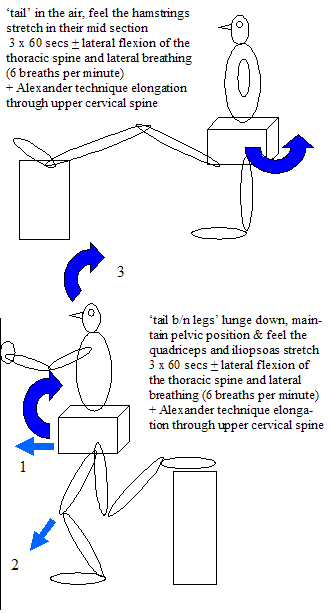
Add thoracic and lumbar spine stretching to the peripheral stretch without losing pelvic neutral
i.e 'don't let the tail wag the dog'
Instructional Design for information on the clinical reasoning process
Treatment
Treatment may consist of
- Hatha Yoga like exercises affecting the thoracic and limbs
- Dry Needling :https://back-in-business-physiotherapy.com/we-do/dry-needling.html
- Muscle Energy Techniques for Pelvic Alignment : https://back-in-business-physiotherapy.com/we-do/dry-needling.html
- Manual therapy techniques including Joint and Neural Mobilisations and Myofascial Releases
- Thoracic Ring relocations : https://back-in-business-physiotherapy.com/we-treat/thorax.html
- Trigger Point Massage : https://www.back-in-business-physiotherapy.com/we-do/trigger-point-massage.html
Link to running shoe advice and feet numbness : Fortunate Feet
external non-sponsored links to Steve Hogg and his business in setting up cyclists at http://www.cyclefitcentre.com/ Sydney Australia
and see non-sponsored link to
local MTB club http://nobmob.com/
http://www.cyclingnews.com for all sorts of advice
Last update : 5 March 2022