Babinski Reflex
by Martin Krause
Clinical Case Presentation : Mrs G
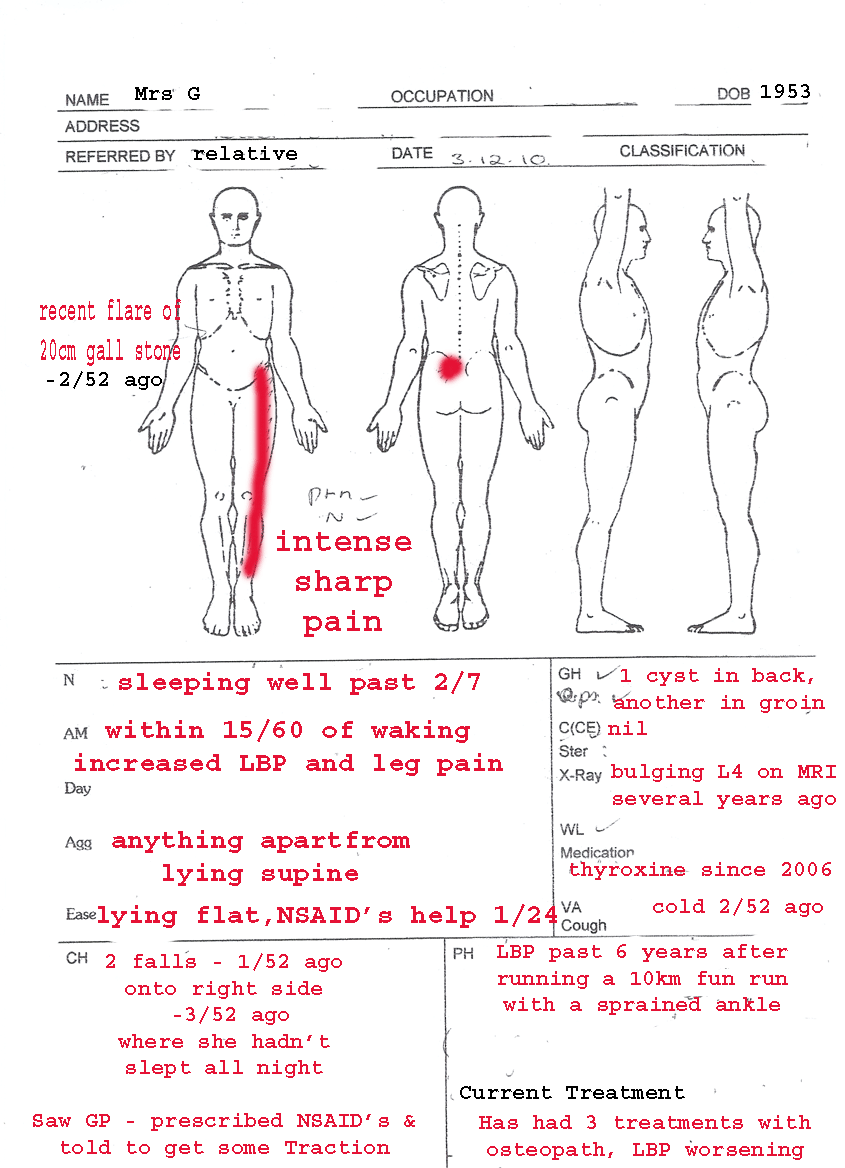
Physio assessment and Treatment
Client presented with no neurological impairments except for a mildly positive left sided Babinski reflex on the medial aspect of the shin and sole of foot
Flexion, extension and lateral flexion were all approx 3/4 ROM. Low Thoracic Spine rotation was restricted to 1/4 to the left and right.
A positive One Leg Stance (OLS) was present on the left suggesting an IntraPelvicTorsion (IPT) right and anterior left hip.
The left hip had 1/2 ROM for ext rotation @ 90 Flex, whereas the right was 3/4. FABERS was 3/4 on left, NAD on right.
SLR with DF was 90 left and right. ASLR painful and positive on left, better with anteriolateral compression of left inferior ribs
Treatment consisted STM to the left anterior hip, adductors and anterolateral abdominal region, joint mobilisations to the left ribs 8 -12 in right side lying and right rotation, dry needling to the left piriformis, MET for anterior rotation of left ilia, MET of T12/L1 into left rotation using the right iliopsoas
Result
About 1/24 after treatment, LBP and leg pain worsened. Went home and drank a whole bottle of red wine. Saw GP next day - prescribed rest and digesic every 4/24, was confident that there weren't any neurological abnormailities. I sent a letter to GP suggesting a mildly positive Babinski along the shin as well as the sole of the foot and that an MRI should be undertaken of the low thoracic and upper lumber spine, as most MRI are taken from L2 downwards. In the mean time she went and saw an acupuncturist.
1/52 later after my treatment an MRI revealed large herniations at the T12/L1 and L1/2 regions. Mrs G saw a surgeon 4 days later and she was operated on 2/7 before Xmas and exactly 2/52 after my treatment.
Comments
Although the treatment was very specific and very gentle a worsening of symptoms did occur. Perhaps fortuitously as a standard MRI would have missed the disc herniations higher up.
On a psychosocial element Mrs G was at the end of a very difficult and extensive house renovation which had been particularly stressful. She was also a fan of osteopathy and acupuncture over physiotherapy. Relatively difficult to interview due to high stress levels just prior to Xmas, and because of the high levels of pain.
Babinski's reflex - Overview
Reflex - Babinski's; Extensor plantar reflex; Babinski's sign
Definition of Babinski's reflex:
Babinski's reflex occurs when the big toe moves toward the top of the foot and the other toes fan out after the sole of the foot has been firmly stroked.
This reflex, or sign, is normal in younger children, but abnormal after the age of 2.
Considerations:
Reflexes are specific, predictable, involuntary responses to a particular type of stimulation.
Babinski's reflex is one of the infantile reflexes. It is normal in children up to 2 years old, but it disappears as the child ages and the nervous system becomes more developed. It may disappear as early as 12 months.
The presence of a Babinski's reflex after age 2 is a sign of damage to the nerve paths connecting the spinal cord and the brain (the corticospinal tract). This tract runs down both sides of the spinal cord, therefore a Babinski's reflex can occur on one side or on both sides.
An abnormal Babinski's reflex can be temporary or permanent.
Common Causes:
* Generalized tonic-clonic seizure (there may be a temporary Babinski's reflex for a short time after a seizure)
* Amyotrophic lateral sclerosis (Lou Gehrig's disease)
* Brain tumor (if it injures or puts pressure on the corticospinal tract)
* Familial periodic paralysis
* Friedreich's ataxia
* Head injury
* Hepatic encephalopathy
* Meningitis
* Multiple sclerosis
* Pernicious anemia
* Poliomyelitis (some forms)
* Rabies
* Spinal cord injury
* Spinal cord tumor
* Stroke
* Syringomyelia
* Tuberculosis (when it affects the spine)
* Reviewed last on: 26/3/2009
* David C. Dugdale, III, MD, Professor of Medicine, Division of General Medicine, Department of Medicine, University of Washington School of Medicine; Daniel B. Hoch, PhD, MD, Assistant Professor of Neurology, Harvard Medical School, Department of Neurology, Massachusetts General Hospital. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
http://www.umm.edu/ency/article/003294.htm
References
Griggs R, Jozefowicz R, Aminoff M. Approach to the patient with neurologic disease. In: Goldman L, Ausiello D, eds. Cecil Medicine. 23rd ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 418.
Hammerstad J. Strength and reflexes. In: Goetz, CG, ed. Textbook of Clinical Neurology. 3rd ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 15.
26 January 2009

























































































































