Neck aetiology, autonomic and immune implications, exercise and diet in the musculoskeletal physiotherapy management of Post Concussion Syndrome (PCS) - a clinical case study with associated research commentary
by Martin Krause, MAPA, Titled member Musculoskeletal Physiotherapy Association of Australia
A 14 year old boy presented to A&E, in August 2016, after receiving an impact to the head during AFL (Australian Rules Football League). Although his SCAT3 scores were relatively mild, he went on to suffer severe lethargy, resulting in a lengthy absence from school, culminating in a return to school for exams in the first week of December 2016. By December, even a 30 minute walk was extremely fatiguing. To place this into perspective, he had been playing elite academy grade AFL for several seasons and was an extremely fit outdoor adventurer.
Confounding Variables :
- end of season injury and hence no follow up from the academy
- suffers from Hypermobile Joint Syndrome (HJS) and possibly Ehlers Danlos Syndrome (EDS), however Beighton score 4/9.
- suffers from food intolerances, particularly to Glutin and diary, but also some other foods. Potential IBS and autoimmune issues.
- had just gone through a growth spurt (190cm)
EDS is considered a soft tissue disease, Additionally, people suffering from EDS frequently have concomitant autonomic dysfunction including POTS (postural orthostatic tachycardia syndrome).
Imaging :
Brain MRI normal
Medical Examination :
Balance remained impaired to tandem walking and single leg stance. The vestibular ocular motor scale showed significant accommodation deficit of 15cm and there was a mild exacerbation of symptoms. ImPACT testing revealed adequate scores and reaction time of 0.65 which is within acceptable range.
History :
School holidays December - January. Return to school and was placed in the lower academic classes. Prior to his concussion he was a top 10 student at an academically selective high school. Took up basketball and rowing as summer sports. Academic results tanked. Several lower limb Basketball injuries (Feb - April 17') as a result of what appeared to be muscular imbalances from the relatively recent growth spurt, as well as taking on a new sport. Showed little interest in returning to AFL as no-one from the AFL academy had followed up on his recovery (or in this case lack of recovery).
Current History :
September 2017 showed a continued decline in academic levels. School teachers noted an inability to concentrate. Academic results still well below pre-concussion levels. Fatigue continuing to be problematic. Stopped going to school for 7 weeks due to another head impact, but this time at Basketball.
Literature Review :
Post Concussion Syndrome (PCS) is defined as "cognitive deficits in attention or memory and at least three or more of the following symptoms: fatigue, sleep disturbances, headache, dizziness, irritability, affective disturbance, apathy, or personality change"
A mechanical disturbance induces a neurological response. A 10-15% neuronal stretching elicits a neurobiological response, including membrane depolarisation (Ca-K flux - increase in intracellular Ca and efflux extracellular K)), shift in intracellular vs extracellular glutamate, which can only be metabolised intracellularly and finally Na/K ATPase is activated to re-establish ionic membrane balance. 80-90% of athletes return to sport within 7-10 days, 2% of this population take over 14 days to recover. Initial symptoms of dizziness tend to a poorer prognosis. Front-back impact seems less damaging than side impact, whereas rotational impact has the worst effect. Neuronal stretching over 20% of it's resting length usually results in complete tear of the neurone (Jane McDevitt and Evgeny Krynetskiy 2017, Concussion, doi: 10.2217/cnc-2016-0020).
Adolescents have been found to have impaired dynamic cerebral autoregulation after concussion that improves along with clinical signs and symptoms in some individuals, whilst remaining impaired in others (Moir et al, 2018 Med Sci Sp Ex,,50, 11, 2192-2199). Moreover, it would appear that measurement of dynamic intracerebral blood flow latency in reaction to changes in position from lying to sitting to standing was more sensitive than static intracerebral blood flow monitoring. This interaction myogenic vasomotor response occurs at a vascular-astrocytic level. Of the 19 people in their investigation, 2 demonstrated complete recovery at 28 days post incident, whereas 7 experienced little change in intracerebral blood flow from the first to last visit (32 + 14 day).
Surprisingly, there appears to be a greater incidence of concussion amongst females (Moir et al 2018; Halstead et al 2010, Pediatrics, 126, 3, 597-615; Dick et al, 2009, Br J Sports Med, 43, Supp, i46-50)
Post concussion dizziness severity predicts step count during recovery. Investigators found that the initial subjective dizziness ratings, but not subjective or objective postural stability measures or overall symptom severity, predict physical activity volume in the subsequent 2 weeks after initial concussion evaluation ( Smulligan KL et al 2022 Med Sc Sp Ex, 54, 6, 905-911). For every one point increase in dizziness rating (range 0->5) there was an approximate 1000 steps/day decrease. Given that exercise volume > 160min/wk is associated with improved post concussion outcomes (Howell DR et al 2021, Am J Sp Med, 49, 7, 1912-1920), dizziness may be limiting factor contributing to non-optimised recovery. Physiotherapeutic intervention including occulomotor training and cervical joint mobilisatons have been advocated for the treatment of dizziness - see below (Reneker JC et al 2017 Scan J Med Sci Sports, 27, 12, 2009-18; Schneider KJ et al 2014, Br J Sports Med,48, 17, 1294-8) ,
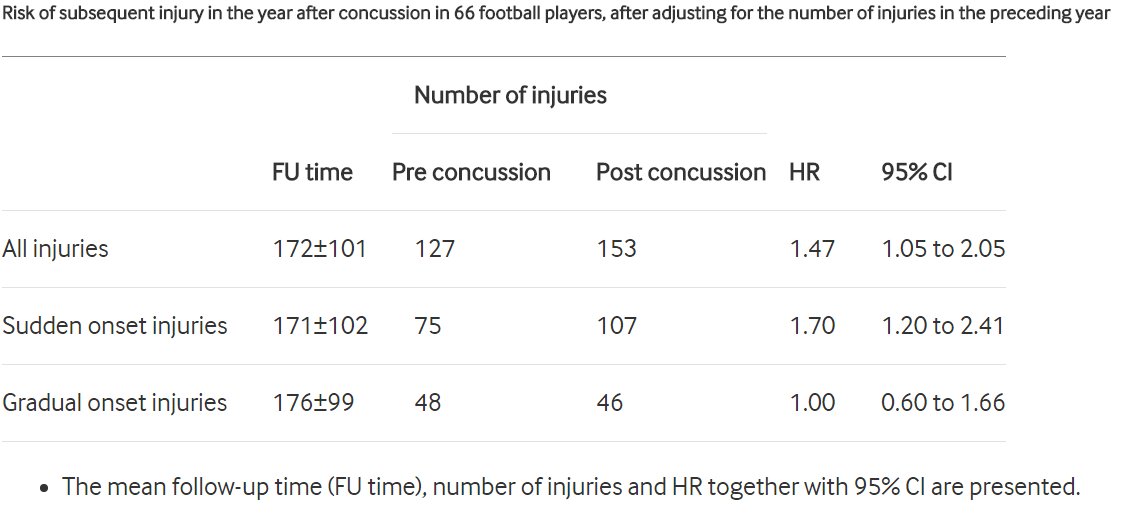
One of the known risk factors for Sport Related Concussion (SRC) is a history of prior concussion (Collins et al 2002. Neurosurgery, 51, 5, 1175-9. Inversen et al 2004, Brain Inj, 18, 5, 433-43). Cumulative effects exist with three or more prior concussions but not with one or two concussions (Inverson et al 2006, 40, 1, 72-75) . Although, most adults recover from concussion after 10 days, there is evidence to suggest ongoing abnormalities in the brain can persist well beyond 10 days (Prichep et al 2013, J Head Trauma Rehabil, 28, 4, 266-273). Thus, with the above described symptoms and potential motor control problems, further complications of PCS also appear to be altered proprioception, an increased risk of musculoskeletal injury which in turn can lead to SRC. The following are the results from soccer players.
Nordstrom et al (2014, BMJ Sports Med, 48, 19, http://bjsm.bmj.com/content/48/19/1447)
Visuomotor reaction time (VMRT) responses and whole body reactive agility (WBRA) have shown neuromechanical deficiencies in elite athletes who reported a history of concussion (Wilkerson et al 2018 Med Sc Ex Sp, 50, 9, 1750-1756). Dual task performances creates competition for neuronal cognitive resources required for higher executive function. Among demands placed by sport on the executive function are visuospatial processing, which can be crucial for management of environmental interactions. Deficits in dual task VMRT have been associated with both a history of concussion and subsequent musculoskeletal injury occurrence.(Wilkerson et al 2017, Cirr Sports Med Rep, 16, 6, 419-427). Sensory organisation test (SOT) balance scores show significant relationships with reaction time and executive function in people suffering concussion (Van der Vegt et al 2019, Med Sc Sp Ex, 51, 2, 264-270). Notably, the ability to use sensory information to adapt motor responses with varying environmental demands is essential for sport safety and performance.
Predictors of PCS are uncertain. However, the following clinical variables are considered factors at increasing risk. These include prior history of concussion, sex (females more prominent), age, history of cognitive dysfunction, and affective disorders such as anxiety and depression (Leddy et al 2012, Sports Health, 4, 2, 147-154).
Genome-wide association study for concussion risk
Genetic polymorphisms in the genes contributing to plasticity and repair (APOE), synaptic connectivity (GRIN2A), calcium influx (CACNA1E), uptake and deposit of glutamate (SLC17A7) are potential biomarkers of concussion incidence and recovery rate (Jane McDevitt and Evgeny Krynetskiy 2017, Concussion, doi: 10.2217/cnc-2016-0020).
Investigators, using a GWA analysis from wo sets of data from the Kaiser Permanent Research Bank (KPRB) and the UK biobank (n=291472 cases), identified two genetic markers as a potential risk factor for concussion (Kim SK et al 2021, Med Sc Sp Ex, 53, 4, 704-711). One of the genes encodes 'plexin' which is thought to transduce signals to steer axonal growth (Jensen et al 2012 Nat Struct Mol Biol,19, 12, 1293-9).
Interestingly, they found that in the RPGEH group being female and weighing less was associated with a greater risk of concussion; whereas, in the UK biobank cohort, they found the opposite, being male, heavier weight and taller resulted in greater risk of concussion. The latter is significant in so far, as other researchers have found increased time to recovery, to baseline sports related concussion, in obese individuals (Lee YM 2016 et al Phys Sportsmed, 44, 3, 217-22).
In this case, he was neither female nor obese, but instead had an athletic morphology. However, at 192cm and 70kg, he had a teenage body whose muscles hadn't filled out into an adult body yet. His head size was large compared to his neck musculature, being a long neck.
Graded exercises
Unlike the 'good old days' which recommended a dark room and rest for several weeks post concussion, the consensus appears to be a graded return to exercise in order to restore metabolic homeostasis. Disconcertingly, highly trained young individuals can find even exercises in bed extremely demanding in the presence of sport related concussion (SRC). Kozlowski et al (2013, J Ath Train, 48, 5, 627-635) used 34 people, whereby 226 days post injury to conclude significant physiological anomalies in response to exercise which may be the result of 'diffuse cerebral swelling'. Researchers have noted lower systolic and higher diastolic blood pressure in PCS (Leddy et al 2010, Clin J Sports Med, 20, 1, 21-27). Due to autonomic dysfunction manifested in altered cardiovascular and pulmonary responses (Mossberg et 2007, Arch Phys Med Rehab, 88, 3, 15-320), whereby some clinicians have recommended the use of the exercise program for POTS (Postural Orthostatic Tachycardia Syndrome). This is a 5 month program which recommends mainly exercise in the horizontal and sitting positions for 1-4 months, including recumbent bike, rowing ergometer and swimming laps or kicking laps with a kick board. Month 4 upright bike and Month 5 upright training such as a elliptical trainer or treadmill. The Modified Dallas POTS Exercise Program can be found here.
Other progressive exercise therapies have also included 20 minutes per day, 6 days per week, for 12 weeks of either treadmill or home gym exercises at 80% of the heart rate at which their concussion symptoms are exacerbated. Their programs were individually modified as the heart rate provoking symptoms increased. When compared to the 'control group', this intervention was shown to improve cerebral perfusion on fMRI, increase exercise tolerance at a higher heart rate, less fatigue and were showing activation patterns in areas of the brain on performing math processing test which were now normalised (Leddy et al 2010, Clin J Sports Med, 20, 1, 21-27).
Graded exercises could also have included 'motor imagery' as espouse by the NOI group and the work of Lorrimer Moseley (University South Australia) when dealing with chronic pain.
Exercise Dose (literature review by Howell et al 2019, Med Sc Sp Ex, 41, 4, 647-652)
- Frequency : 5d/wk of moderate intensity or > 3 d/wk of vigorous intensity
- Duration : 30-60 minutes/day (150min/wk) at moderate intensity or 20-60 minutes (75 min/wk) of vigorous intensity
- Mode : exercise using major muscle groups eg walking, jogging, cycling or swimming
- Volume : > 500-1000 MET/min/wk (MET = 3.5 ml O2/kg/min)
- Pattern : exercise is performed ideally in one continuous pattern; however multiple sessions of > 10min can be performed to accumulate the desired total duration and volume of exercise
- Progression : Gradual progression of exercise volume by adjusting duration, intensity and/or frequency is recommended to gain continued aerobic fitness improvements
Ongoing Symptoms :
The literature review by Leddy et al (2012) found that ongoing symptoms are either a prolonged version of concussion pathophysiology or a manifestation of other processes, such as cervical injury, migraine headaches, depression, chronic pain, vestibular dysfunction, visual disturbance, or some combination of conditions.
Anatomical considerations :
Extensive anatomical connections between the eyes, neck and vestibular system (Wallwork et al 2007, JOSPT, 37, 10, 608-612) allow sensory information from neck proprioceptors to be processed together with vestibular information which, via the lateral vestibulo-spinal tract, affect the control of postural muscles such as the deep trunk muscles (Hain 2011, Neuro-Rehabilitation, 29, 2, 127-141).
Psychological considerations :
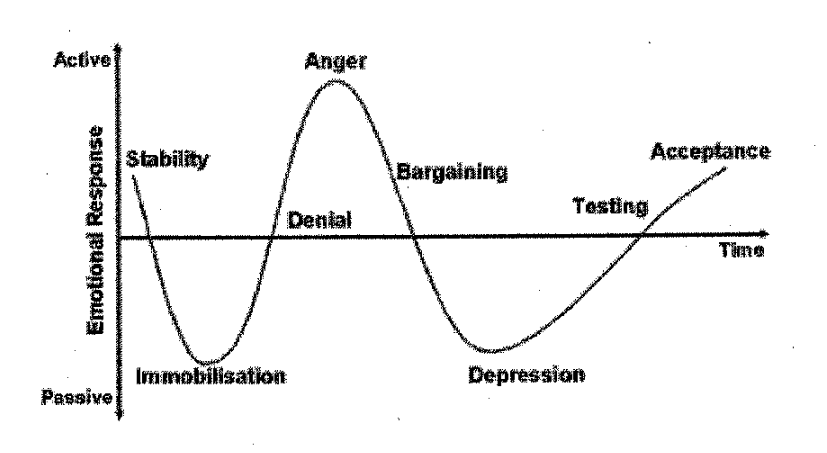
The Kubler Ross model of grief are applicable when it comes to chronic sports injuries.
Mental health among athletes is an important consideration that has recently gained more attention. The 2019 International Olympic Committee (IOC) consensus statement on mental health in athletes reported on the high prevalence rate of mental health symptoms in athletes and the relationship of mental health with physical injury and subsequent recovery (Reardon CL et al 2019 Br J Sports Med. 53, 11, 667–699). The IOC urged that mental health is a vital component of athlete well-being and cannot be separated from physical health. Assessment of mental health and subsequent management should be a routine part of the medical care of athletes. The IOC also concluded that cognitive, emotional, and behavioural responses are important factors in injury outcomes, and mental health disorders can complicate recovery. A systematic review of 28 studies reported 65% of those patients not returning to play cited a psychological reason for not returning (Nwachukwu, BU et al 2019 Orthop J Sports Med. 7, 5, 23259 67119845313). Fear of reinjury, lack of confidence in the knee, and depression were the most commonly cited psychological reasons.
Physiotherapy Assessment :
One year PCS, fatigue continued to persist. Cognitive deficits with school work were reported to becoming more apparent. Assessment using various one leg standing tests employing oscillatory movement around the hips and knees for kinetic limb stability and lumbopelvic stability, which had been employed 6 months previously for his Basketball injuries were exhibiting strong deficits, despite these being 'somewhat good' previously.
Significantly, during the acute phase of SRC, rugby union and rugby league players have been seen with alterations of both balance strategies and motor control of the trunk (Hides et al 2017, Musculoskeletal Sci Pract, 29, 7-19).
Investigators (Lempke et al 2020, Med Sc Sp Ex, 52, 8, 1650-1657) comparing clinical reaction time (RT) assessments with functional RT found little correlation. Clinical RT assessment included computerised evaluation of simple and complex RT, Stroop RT, composite RT and Drop Stick. Functional assessment included gait, jump landing, single-leg hop, anticipated cut and unanticipated cut. This implies clinicians may not be sensitive to the functional RT required for safe and effective sports participation, potentially leading to further musculoskeletal injury, during post concussion return to sport. Interestingly, they found dual task RT quite sensitive to physical and cognitive deficits. A sweet spot may exist for dual tasks between those which are too easy (hockey puck drop stick) and those which are too hard (unanticipated cutting). Furthermore, they observed that the single leg hop RT may be a very useful test, as the transition from a dynamic movement to a static position is a relatively unaccustomed and hence un-practiced task, thereby minimising deficit masking through learning effects.
Physical Examination : cervical and thoracic spine
Due to the Joint Hypermobility Syndrome (JHS) it was difficult to ascertain neck dysfunction based on range of movement testing. ROM were unremarkable except for lateral flexion which demonstrated altered intervertebral motion in both directions. Palpation using Australian and New Zealand manual therapy techniques such as passive accessory glides (upslopes and downslopes and traction) exhibited muscles spasms in the upper right cervical spine. In particular, the right C1/2 regions demonstrated most marked restrictions in movement. Eye - Neck proprioceptive assessment using blind folds and laser pointer also revealed marked variance from the normal. Repositioning error (RPE) using the laser pointer with rotation demonstrated marked inability to reposition accurately from the left, tending to be short and at times completely missing the bullseye. Gaze stability with body rotation was NAD. Gaze stability whilst walking displayed some difficulty. Laser pointer tracing of the alphabet was wildly inaccurate and cognitively demanding. Thoracic ring relocation testing also revealed several anomalies, which may have also accounted for some of the autonomic dysfunction observed.
Occulomotor assessment and training
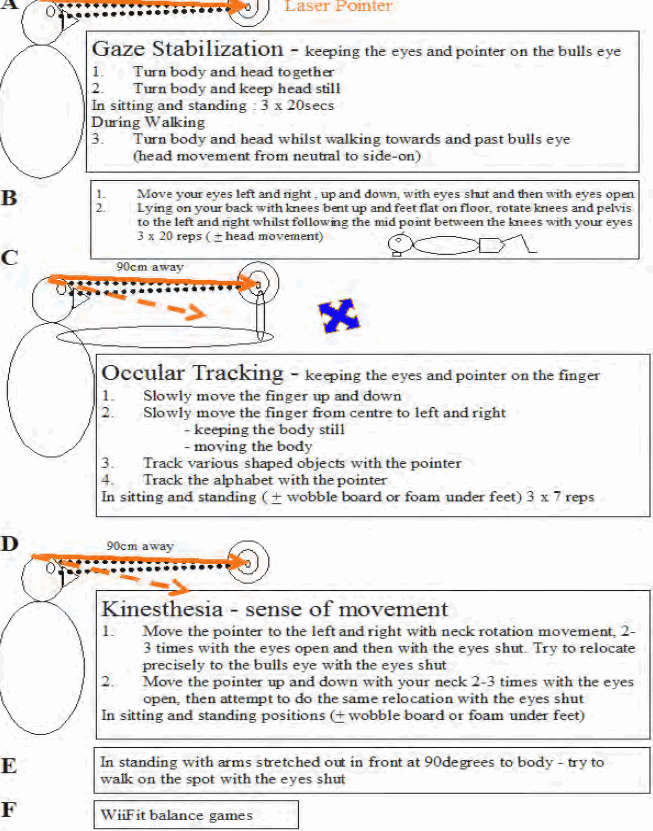
Upper Cervical Spine :
The upper cervical spine (atlas and axis) represents approximately 50% of the available rotation. An investigation into the environmental and physiological factors affecting football (soccer) head impact biomechanics found that rotational acceleration was one of the few factors approaching significance and concluded that more research should be undertaken to evaluate this (Mihalik et al 2017 Med Sc Sp Ex, 49, 10, 2093-2101).
Headache :
Commonly referred to as cervicogenic headaches, one in five headaches in the general population are thought to be due to the cervical spine. The Upper Cervical Spine is particularly vulnerable to trauma because it is the most mobile part of the vertebral column, with a complex proprioceptive system connecting the vestibular apparatus and visual systems. It also coincides with the lower region of the brainstem and fourth ventricle. The brainstem houses many neurones associated with autonomic responses to pain and balance. Imaging of the fourth ventricle for swelling of the 'tonsils' and Arnold Chiari malformations are recommended when symptoms persist. In particular, children and adolescents are more vulnerable to neck contusions due to the proportionately larger head and less developed musculature. Cervical vertigo and dizziness after whiplash can mimic symptoms of PCS.. Mechanoreceptor dysfunction and vertebrobasilar artery insufficiency should be part of the differential diagnosis. Mechanical instability of the Upper Cervical Spine should also not be missed.
Further Interventions :
Neurocognitive rehabilitation of attention processes. Psychological intervention using cognitive behavioural therapy (CBT). Neuro-opthalmologist to assess and treat smooth pursuit eye tracking. Naturopath for food intolerances and dietician for the optimisation of diet.
Diet :
In cases with chronic fatiguing factors, nutrition can be become a vital aspect into the reparative process. This may include energy and mineral rich foods such as bananas, green leafy vegetables for iron and magnesium (200-300mg), oranges for vitamin C (anti-oxidant and helps with the absorption of iron), anti-oxidant rich foods such as EPA/DHA (1000mg) fish oil, curcumin (Tumeric), Cats Claw, Devils Claw, Chia seeds, fruits of the forest (berries), and CoQ10 with Vitamin B. Folate and Ferritin levels should also be checked. Calorific energy intake should balance with energy expenditure. However, as we are often dealing with young individuals, as in this case, some form of comfort food may be appropriate such as, nuts, legumes, homus and sushi. Protein intake prior to carbohydrate intake may help ameliorate any blood sugar fluctuations due to Glycemic Index factors, however simple carbohydrates (high GI) should be avoided wherever practical. Even oats need to be soaked overnight and cooked briefly, otherwise they become a high GI food and may even affect the absorption of iron. The type of rice used can also influence GI, hence the addition of protein such as fish. Protein supplementations are generally over-used. Daily protein intake should not exceed 1.2g per kg of body weight per day. Dosage for children is less than that for adults.
See Nutritional Section of this Site
Probiotics such as Sauerkraut should also be considered when dealing with potential immune disorders related to the gut. In this case IBS was a confounding variable in his presentation. The amount of human DNA is totally under-whelming compared to that of the intestinal mircobiome. The intestine is composed of a complex ecosystem of more than trillions of bacteria, viruses, fungi, Protozoa and Archea that live in a symbiosis with the host in the gut lumen. The healthy microbiome include a limited number of highly represented taxa, such as Bacteroides and Prevotella and a large number (>2000 to date) of minor players with low representation but high metabolic activity. These latter 'players' with high metabolic activity are likely to be the ones which interact with the musculoskeletal system. In older age, species richness and diversity of the microbiome decline, inter-individual variability increases, and resilience to perturbations are reduced. Apart from aging, the presence of acute and chronic diseases affects the microbiome. In the aging and/or unhealthy microbiome a 'dysbiosis' can occur, where a disruption of the gut balance 'symbiosis' results in intestinal permeability, allowing bacteria, or bacterial toxins and metabolites to enter the host circulation thereby promoting sub-clinical inflammation. Clinically, sub-clinical inflammation has been referred to as 'inflammaging' and 'immunosenescence'. Further research on metabolic immune reactions can be found elsewhere on this website.
Trunk muscles :
Researchers have found that a history of SRC had an increased possibility of having altered size and contraction of their trunk muscles, including smaller multifidus, larger quadratus lumborum muscles, and asymmetrical contraction of their transverse abdominis muscles, whereby an increased thickness and resting tone of the right anteroloateral abdominal muscle has been observed (Hides et al 2017 Med Sc Sp Ex, 49, 12, 2385-2393).
In this case, by the second incident (Basketball impact), the subject was 15 years of age and 193cm in height. Apart from being very tall for his age he also has joint hypermobility. Combinations of SRC, growth spurt and hypemobility may have had a greater impact on his motor performance making secondary trauma more likely? A 3-6 increased risk of future SRC has been reported in the literature in cases of concussion (Abrahams et al 2014, Br J sp Med, 48, 2, 91-97).
In our subject, using the laser repositioning error described above, marked inability to reposition the neck from the left was seen. This concurs with the findings in Australian Football Players (AFL), where a mean of 4.5 degrees of joint position error was reported on the left hand side (Hides et al 2017 Med Sc Sp Ex, 49, 12, 2385-2393). This is noteworthy, as our subjects initial concussion took place during AFL, with the subsequent concussion occurring in Basketball.
It should also be remembered that this subject presented to physiotherapy for an ankle injury some 6 months after the initial concussion. Lower limb kinematic exercising ability, emphasising global balance and kinematic 'inverse dynamics' muscular energy strap transfer principles, demonstrated strength and balance deficits within the following programme.
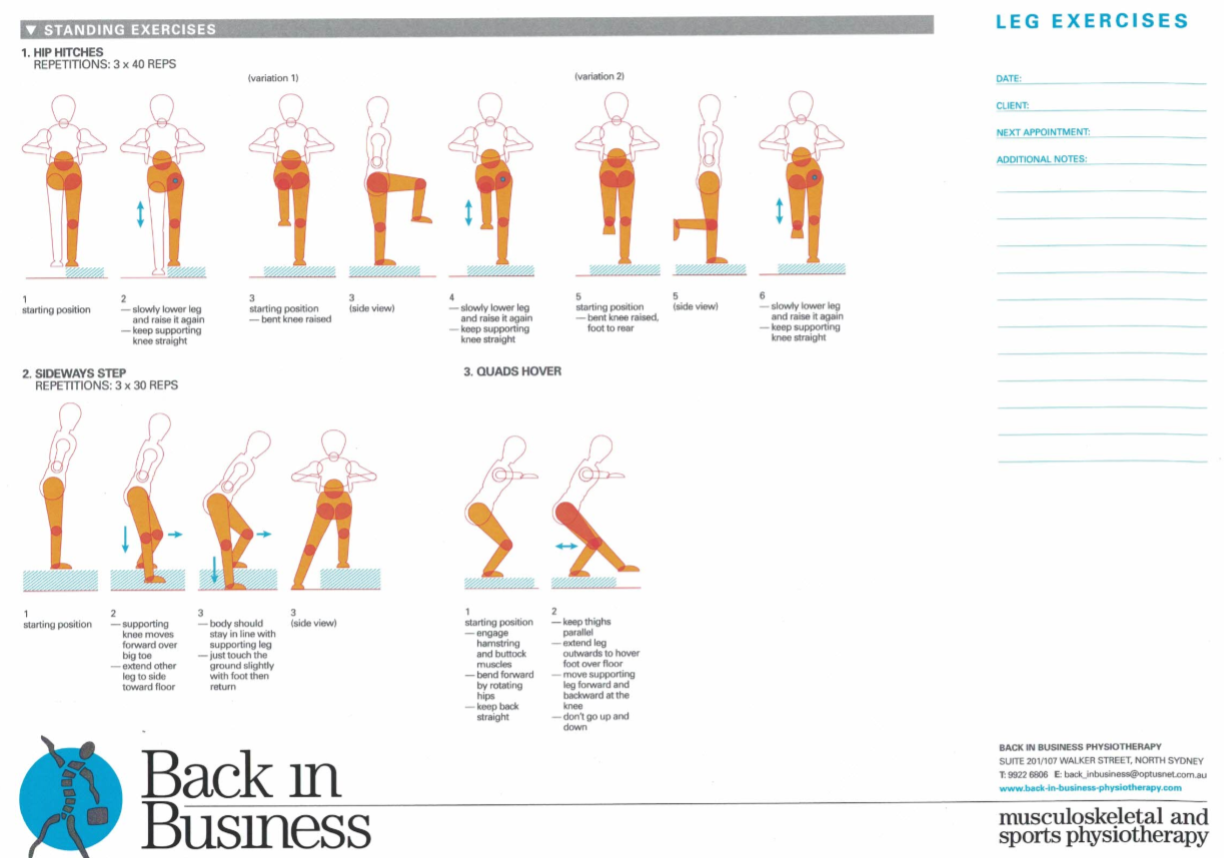
Leaning forward, pivoting through the hip in exercise 2 and 3, will lead to better hamstring, gluteal and quadriceps engagement. The Sideways Lunge should only be down once the Reverse Lunge is perfected. The use of a slider on the floor and progressing from reverse lunge, to diagonally sideways lunge and eventually sideways lunge may need to proceed lunges with steps and certainly forward lunges. Aim, is to re-orient the motor learning systems to efficiency of movement both metabolically and mechanically.

It should be noted that this regime places emphasis on repetitive loading; hence 3 x 40 reps.
Interestingly, an investigation comparing lower limb (LL) and back exercises (lumbar extension LE and lumbar stabilisation LS) for runners with chronic low back pain reported
- greater improvement in self-rated running capability and knee extension strength in the LL group vs LE and LS groups
- greater increase in running step length in LL and LE groups and
- similar reductions in running induced pain and improvement in back muscles across all three exercise groups. (Cai et al 2018, Med Sc Sp EX, 49, 12, 2374-2384)
Extrapolation of these results to the current clinical setting suggests the importance of lower limb dynamic stability in cases of concussion. Moreover, recognition of these deficits may have prevented the second incidence of concussion?
Exercise and cognition
Corpo Sano Mente Sana or a Healthy Mind in a Healthy Body, has been the mythical connection between brain and brawn. In terms of neurophysiology, the dopaminergic system has been attributed for the drive to exercise. Habitual exercisers have been shown to have been predicted to have greater prefrontal cortex (PFC) executive function. Investigators have found a link between 'blink rate' and cognitive function on STROOP testing and functional near-infrared spectroscopy (Kuwamizu R et al 2021, Med Sc Sp Ex, 53, 7, 1425-1433).
Orienteering is a sport requiring high endurance physical fitness, agility and high cognitive function, as the task demands navigation, at speed, through unknown terrain. In terms of this clinical presentation, he commenced a programme of multi-day bushwalking/backpacking approximately 2 years after the initial concussion incident. Later, he participated in orienteering and rogaining events.
Further reading on higher executive function, clinical reasoning and learning using orienteering as a construct can be found elsewhere on this website : https://www.back-in-business-physiotherapy.com/physiotherapy-teaching/constructivism.html
Conclusion
Investigations, into people with persisting PCS, demonstrated that they applied more force over time to control balance. Helmich et al (2016, Med Sc Ex Sp, 48, 12, 2362-2368) proposed that in regard to cognitive processes, the increase of cerebral activation indicates an increase of attention demanding processes during postural control in altered environments. This is relevant in so far as individuals with post concussive symptomatology have a variety of symptoms including headache, dizziness, and cognitive difficulties that usually resolve over a few days to weeks. However, a subgroup of patients can have persistent symptoms which last months and even years. Complications in differential diagnosis, can arise clinically, when neck dysfunction and altered motor control occur concurrently due to both neck and cerebral pathology. For example, Whiplash and other traumatic head and neck injuries can result in pathology to both regions, whereas, more discreet altered cognitive processing from concussion can result in altered neck motor control. Musculoskelatal Physiotherapy can play a vital part in the treatment of neck dysfunction including the re-establishment of occulomotor proprioception and managing localized strength and cardiovascular exercise regimes. A total body, multi-disciplinary approach which is well co-ordinated amongst practitioners is vital to an optimal outcome.
Final Outcome
In 2021, some 5 years after the initial concussion at the Sydney Swans Academy, his status was as follows
- 20 years of age
- never went back to AFL or any type of contact sport
- missed 1.5 years of school (2016 and 2017)
- did his matriculation year (2019) almost solo in the library after school, (where he also happened to meet his current girl friend) whilst using class time for revision. Dropped mathematics, as it was a subject which needed continuous learning and the gap of 1.5 years was too much to catch up on. Managed to get a top 10 result in the State for Geography and an overall ATAR of 97%.
- 5 years post concussion studying environmental science/law at Sydney University. Caught up on Calculus and Statistics during summer semesters at University
- taken up rock climbing, bouldering and surfing (2020).
- 3 - 4 years post concussion multi-day bushwalking in Tasmania, orienteering and rogaining
- still has some issues with concentration when fatigued
- avoids alcohol or anything else which he feels has an impact on his brain.
- still prone to hypermobility joint strain issues
- in 2023 we pack rafted the Atlanta River in Alaska and climbed into the Arigetch Peaks of the Brooks Range during a 23 day expedition - see elsewhere, on this website, for photos of trip.
See link to repetitive linear head trauma (heading at soccer) for more information :
https://www.back-in-business-physiotherapy.com/latest-news/264-repetitive-linear-head-trauma.html
Updated : 20 April 2024.
Original : 17 November 2017