There are many aetiologies of shoulder pain. The most common shoulder complaint is what is commonly referred to an an 'impingement syndrome' where immune-metabolic changes within the substance of the tendon of the supraspinatus (rotator cuff) muscle and subacromial bursa create a 'painful arc' when lifting the arm above shoulder height (this usually occurs in the ranges of 70 - 120 degrees). Other pathology includes subscapularis tears from anterior dislocation of the shoulder, biceps tendon issues and posterior shoulder capsule tightness with weakness of the rotator cuff. Additional problems may arise with the acromioclavicular and sternoclavicular joints as these are the joints connecting the shoulder blade, via the bony strut (collar bone) to the skeleton. These shoulder pathologies may need differential diagnosis with referred pain and weakness from neck and thorax pathology.
Posterior shoulder dislocation
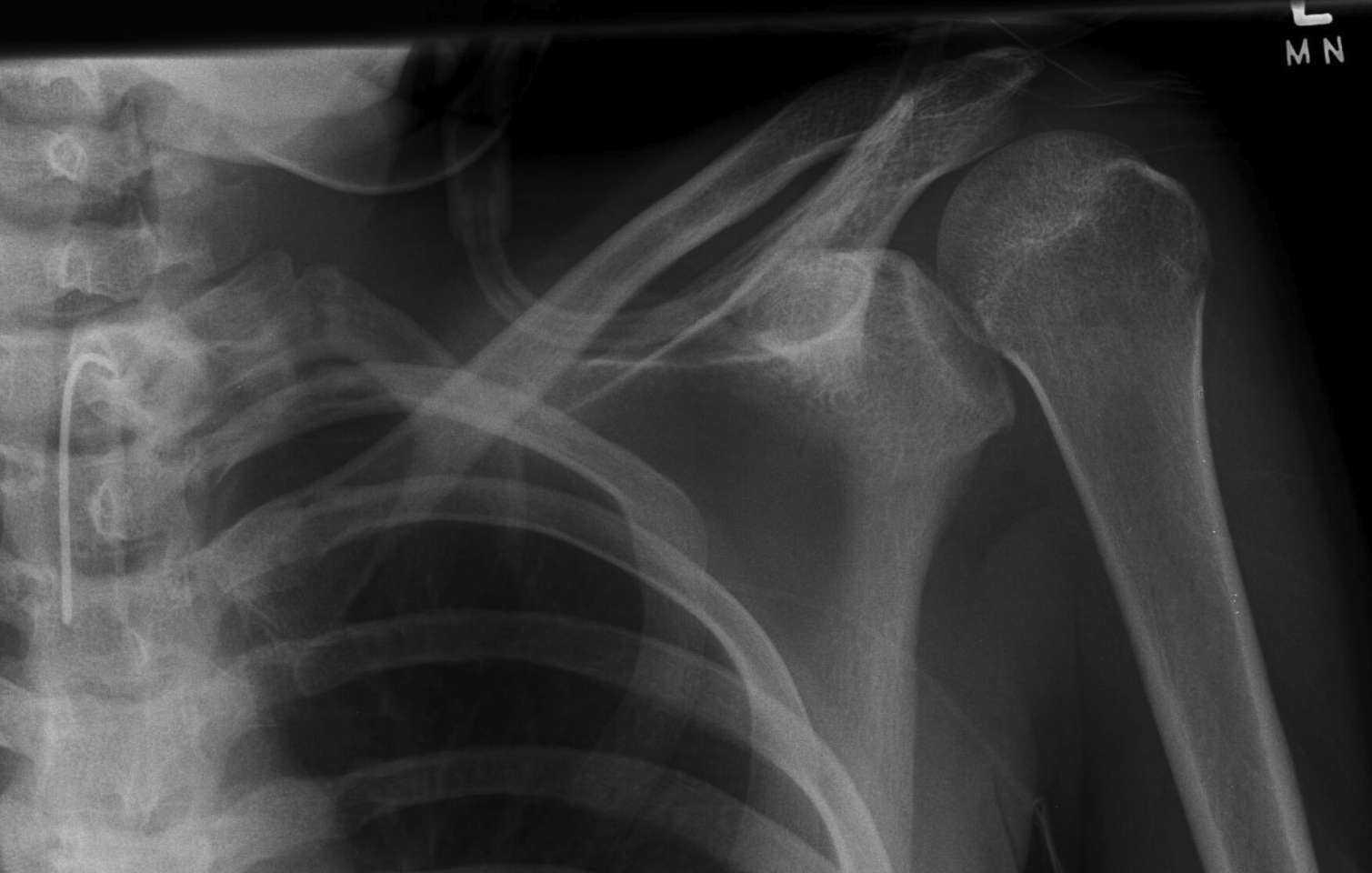
Biceps tendon pathology
- according to Dr Stephen J O'Brien MD, MBA (2011), the O'Brien's test is 88% positive for an incarcerated long head of biceps tendon and only 54% have a labral tear, whereas the Subscapularis is usually normal in 300 cases.
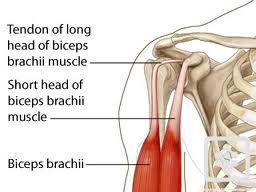
- 63.6% of people under 40 will complain of fatigue discomfort, whereas 42.1% between the ages of 40 and 60 will complain of this when dealing with an 'incarcerated biceps'.
- "3 Pack" examination
"extra-articular"
- direct palpation of bicipital groove
- throwing test
"Intra-articular"
- active compression test
- 90 abd ER isometric test -> palpate biceps tendon in bicipital groove if pain anterior it's a tendon problem, if the pain is posterior then it is likely to be internal impingement
- tightness of the posterior capsule will cause the head of the humerus to migrate superiorly during abduction and external rotation resulting in subacromial impingement. Subacromial impingement is where the bursa and rotator cuff impinge between the humeral head and acromion. Frequently people have pain at night. Hawkins test can be preformed with isometric internal and external rotation to confirm a 'working hypothesis' of subacromial issues. MRI can further add diagnostic weight if not all of the three clinical signs are present
- rotator cuff tears (R.C.T) increase in frequency with aging (20% in 30-39 year olds, 60% in 60-69 year olds and 80% in 70-79 year olds) (Julie R Walton PhD 2011). Young tendon fibroblasts have a progressive collagen cross-linked matrix. There is very little renewal of collagen after 30 years of age. Tendon trauma causes the induction of protein kinases resulting in cell apoptosis (programmed death). This can be seen around small blood vessel proliferation. Hypoxia induces type III collagen production which appears to be driven by immune inflammatory cytokinase markers such as IL I, IL6, IL8, MCP-1. This process has been referred to as a "Collagen Switch" (George Murrell 2011). Additionally, there seem to be some markers associated with lipid metabolism which drive degenerative tendonopathy, suggesting people who are over-weight or who have metabolic syndrom (hyperlipidemia, diabetes) may be more susceptible to tendonopathy
- the supraspinatus muscle architecture means that the tendon is more likely to degenerate on the subsurface i.e. adjacent to the head of humerus. Mid substance and superior degeneration can also occur but less frequently.
- three predictive tests for R.C.T's are supraspinatus weakness, weakness in external rotation, impingement pain in external rotation and/or internal rotation. Full thickness tears of <2cm2 are considered small, 2-4cm2 large and >4cm2 are 'massive and irreparable' (Prof George Murrell 2011).
- shoulder instability can occur when the intra articular pressure of -40cmH2O (ie the vacuum) is disturbed. Clinically, they present with increased strength of the external rotators over the internal rotators (normally ER strength is 60% of IR, whereas with anterior instability the ER strength is 85% of IR strength) (Eiji Itoi, MD, PhD Sendei, Japan 2011). In 0 degrees the Superior Glenohumeral ligament acts as a stabiliser, at 45 degrees abduction it is the Mid GHL and at 90 degrees the inferior IGHL. The latter acts as a hammock for the humerus. For this reason proprioceptive isometric stabilisation exercises of the subscapularis and infraspinatus with the arm resting on table at 90 degrees abduction is considered important in the rehabilitation of the throwing arm. Remember the rotator cuff muscles blend with the ligaments except at the foramen of Weitbrecht. Even at 45 degrees abduction O'Brien considers the Ant IGHL as the primary restrainer.
- Frozen shoulders also known as adhesive capsulitis are frequently of unknown aetiology. However, people with diabetes or hyperlipidemia have an increased tendency towards frozen shoulders due to the effect on the blood vessels of the suprascapula nerve as well as the direct effect on tendon metabolism. Immune compromise in for example people with severe neutropenia are also more susceptible to frozen shoulder. Post traumatic inflammation is also a potential contender to set the scene for a frozen shoulder. Moreover, there frequently appears to be a familial tendency in it's aetiology. People with Dyputrens contractures tend to have more severe problems. The severe acute painful stage can last from 6 weeks to 6 months. The 'cold' frozen stage can last up to 18 months. Cortisone can in some cases help with pain in the acute phase. Hydrodilation is sometimes used in the 'cold' frozen stage. People frequently find a lot of comfort using a hot pack in the arm pit. High doses of fish oil using 3000mg of EPA/DHA have been advocated. Physiotherapy includes a multimodal approach such as dry needling, laser therapy, soft tissue massage, joint mobilisations of the shoulder, ribcage, spine and a series of exercises.
Altered biomechnical conditions are a result of misuse, disuse, abuse whose damage causes a reciprocating viscious cycle of muscle-tendon atrophy, degenerative changes, and immune-metabolic dysfunction. At Back in Business Physiotherapy we use a combination of 'hands-on' therapy, exercise and nutritional supplementation to optimise the rehabilitative process.
Immunological factors as a result of disuse
A biphasic stress response has been described in muscles during 'reloading' after a period of 'unloading'. Mechanical unloading as a result of disuse results in substantial muscle atrophy. This atrophy is a result of both increased protein degradation and reduced protein synthesis. Signaling pathways leading to this, include oxidative stress, proinflammatory signaling, reduced stress response, including heat shock proteins (HSP) and insulin-like growth factor (IGF-1). Insufficient HSP and antioxidant enzymes elicits oxidative damage of proteins and lipids (Lawler et al 2003, Free Radic Biol Med, 35, 9-16). Hence, unloading elevates oxidative stress. Paradoxically, loading also elevates oxidative stress. Nuclear Factor kB (NF-kB) has been implicated in both processes. During unloading it is thought to induce numerous pro-inflammatory genes including nitirc oxide synthase, cytokines, ubiquitin pathway ligases as a result of withdrawal of the stress - response including HSP25, HSP70, IGF1/Akt pathway (Lawler et al 2006, Muscle Nerve, 33, 200-207). The early portion of reloading, after a period of immobilisation is characterised by muscle damage and inflammation which requires a cognitive approach using a realistic time-frame for recovery to take place. although, muscle recovery after 7-10 days of unlaoding is rapid (7 - 9 days), prolonged immobilisation greater than 17 days exhibits impaired recovery of muscle mass (Kasper 1995, J Appl Physiol, 79, 607-614). Reloading of muscles have been shown to result in a large up-regulation of NF-kB DNA-binding activity (Lawler et al 2012, Med Sci Sp Ex, 44, 4, 600-609). HSP25 phosphorylation decreased during prolonged unloading but returned to normal after 28 days of reloading. HSP70 and IGF-1 remained depressed during short term reloading but returned to normal levels as muscle mass improved, whereas in contrast Akt phosphorylation was greater in short term reloading but returned to normal by day 28 (Lawler et al 2012).
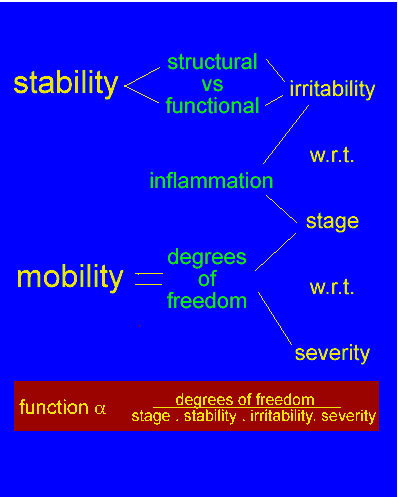
Joint stability in the shoulder
- biomechanics and gamma reflexes
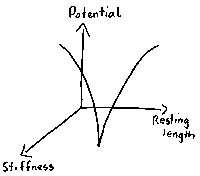 |
Joint stability is determined by the muscular stiffness in 'soft' joints such as the neck knee and shoulder. Muscular tension generates stability at the glenohumeral jnt the outward curves represent the stabilising influence when the prime mover muscles act on the shoulder |
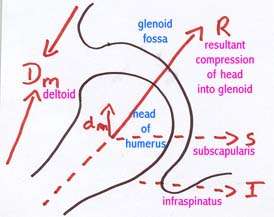 |
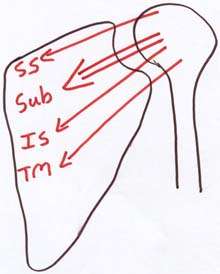 |
To enable stability at the glenohumeral joint during arm elevation the scapula muscles position the glenoid to provide optimal orientation for the rotator cuff stabilising function |
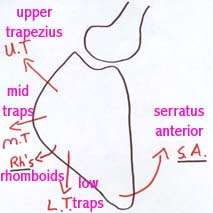 |
|
If the rotator cuff and scapular muscles do not operate synergistically then the potential for glenohumeral subluxation & subacromial impingement is generated |
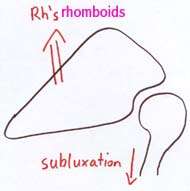 |
|
Thorax
Patients frequently seek treatment for pain in various parts of the body, but infrequently present for treatment of thoracic pain. Yet, simple, quick assessment and correction of the thoracic rings frequently demonstrates a link to the pain and musculoskeletal dysfunction in areas some distance away. Wainner et al (J orthop Sports Phys Ther, 2007; 37, 658-660) describe regional interdependence as “the concept that seemingly unrelated impairments in a remote anatomical region may contribute to, or be associated with, the patient’s primary complaint.” This perception suggests that interventions targeting adjacent anatomical areas may directly affect the outcomes of the involved joint. Boyles et al (Manual Therapy, 2009 Aug;14(4):375-80) and Strunce et al (J Man Manip Ther, 2009, 17(4): 230-236) have demonstrated the immediate effects of thoracic spine thrust manipulation on patients with shoulder impingement syndrome. The latter describing a 51% reduction in shoulder pain, 30-38 degree increase in range of motion (ROM), and a mean patient perceived global rating change of 4.2 in 21 subjects. McCormack (J Man Manip Ther., 2012 Feb;20(1):28-34) showed a 25 degree improvement in shoulder ROM when using thoracic spine manipulation in the treatment of adhesive capsulitis. Brian Mulligan described 'mobilisation with movement' (MWM) techniques on the first rib which have dramatic effects on the cervical ROM for contralateral lateral flexion and ipsilateral rotation. Canadian physiotherapist Linda Joy Lee has advocated ring shift corrections for low back pain, pelvic girdle pain and hip problems, as well as shoulder and neck issues.
Interested readers should look at the thorax apsect of this website.
Summary
- the rotator cuff muscles provide glenohumeral stability
- the scapular muscles provide the positioning for inferior stability of the glenoid labrum for a snug fitting humeral head
- with the deep joint stabilizing muscles providing the stability, the prime movers may provide the 'action'
- generally speaking the stabilizing muscles of most joints are one joint muscles with an endurance function; whereas the prime movers are the muscles which lend power to the movement e.g. Pectoralis Major. Therefore when designing an exercise regime the client must begin with good muscular stability before commencement of training of the prime movers.
- Frequently, clients compensate for lack of stability by increasing the speed at which they do the task. This then leads to further in-coordination, poor timing between muscles, loss of synergy, and more dysfunction.
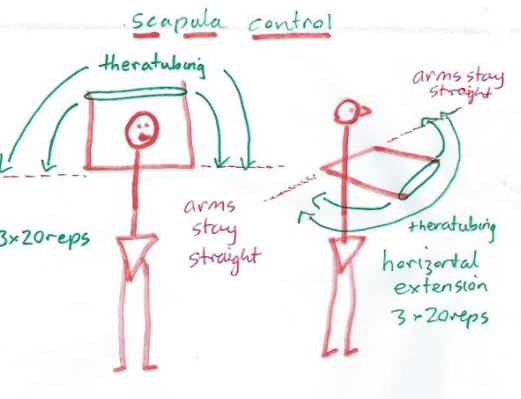
- Closed kinetic chain training to gain scapula and rotator cuff stability may encourage gamma afferent feedback from the annulospiral endings, as well as activate the nuclear bag and nuclear chain fibres
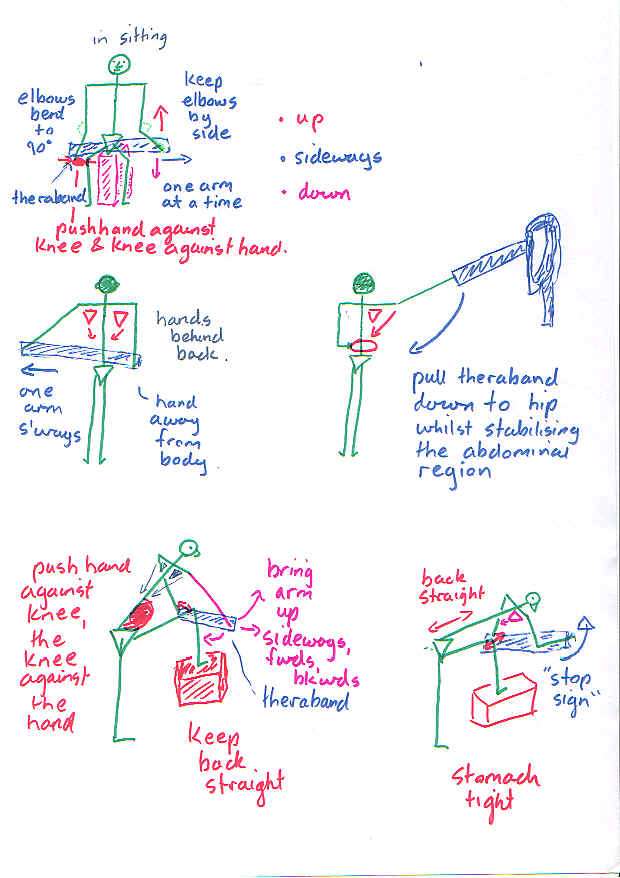
- Plyometric type exercises using theraband are designed to encourage eccentric-concentric control of the prime movers.
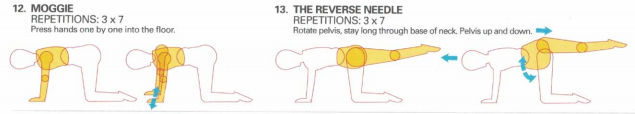
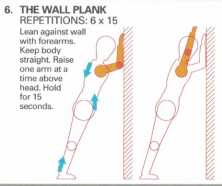
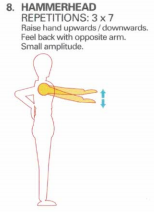
Oscillations in another part of the body can be used to establish harmonic frequency elsewhere. For example, arm movements activating the opposite erector spinae activity, pelvic oscillations for scapular control, arm lifts for contra-lateral gluteal activity.
Alternate kneading of the hands into something soft activates the abdominal muscles, spinal rotatores and scapula muscles. Oscillations of the pelvis around the hip activates eccentric scapula control.
Alternate lifting of the arm off the wall activates the opposite buttock muscle.
Alternating arm flexion/extension around the 90 degree angle activates the opposite erector spinae muscles of the low thorax and upper lumbar spine. Moving through the horizontal with a consistent oscillation also has varying effects on those muscles.
Importantly, if loading is required to activate a muscle building response, then repetitions need to include tremor. Either fine motor tremor or exhaustion tremor, if we want to include a 'deterministic chaotic variable', which it is hypothesised to create an immune training variable. Interested readers, on chaos, should view https://www.back-in-business-physiotherapy.com/health-advocacy/exercise-and-the-immune-system-during-covid-19.html
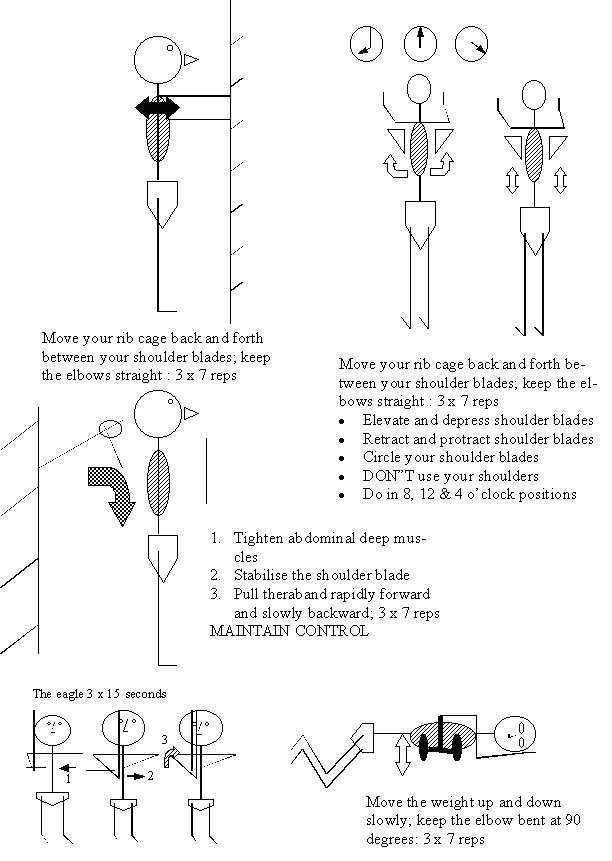
Closed kinetic chain exercises 5, 8-13, promoting stability. Should be done slowly, as the deep stabilising muscles are red slow twitch muscle fibres. Such exercises combine the shoulder, neck, shoulder blade, thorax and pelvic complex to functionally stabilizing activities. Moreover, Swiss Ball Exercises in 2 and 4 point Kneeling can be used to promote over-shoulder-height arm activity whilst having the arms below the shoulders!!! Apart from the Prone Roll, the Swiss Ball can also be used to do diagonal upward rolls as well as prone scissors. Open chain dynamic exercises can eventually be incorporated whilst kneeling on the Swiss Ball
Plyometrics - open kinetic chain
Open kinetic chain exercises are essentially less stable than closed kinetic chain exercises. They fall into two essential categories - those which pull inward and hence energy towards to body and those wish pull away. Basically, hypermobile people need to focus on stability, perfecting closed kinetic chain exercises, moving on to a hybrid of closed kinetic chain with open kinetic chain pulling inwards and eventually adding the open kinetic chain pulling outwards.
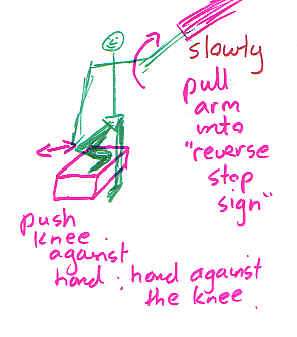
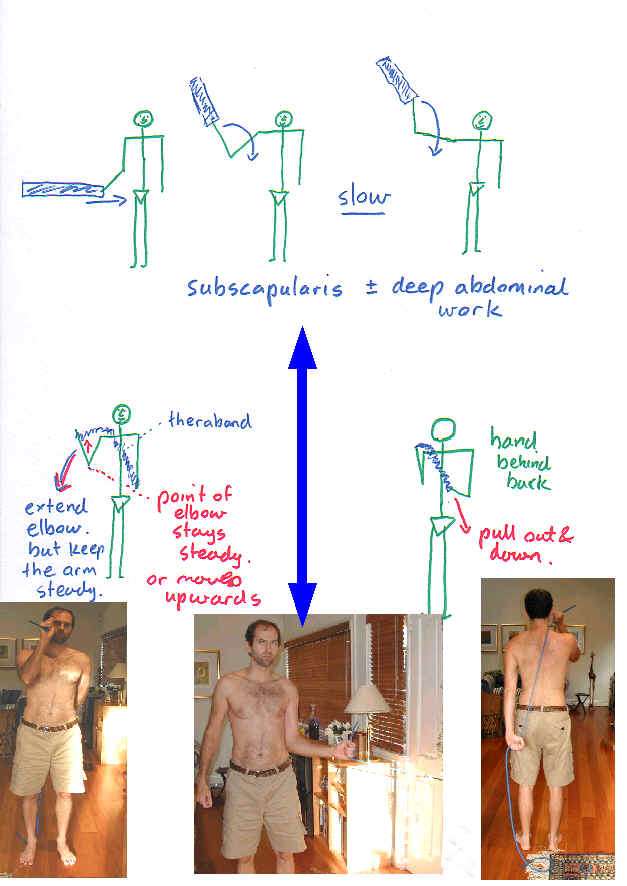
Care needs to be taken with the open kinetic chain internal and external rotation as it's not uncommon to aggravate the transverse ligament and long head of biceps with this exercise. Additionally it isn't a very functional exercise. Exercises that more closely mimic the activity to which the person needs to return to, will generally be more effective, as well as present an opportunity to use the exercise as a metric on the path to recovery.
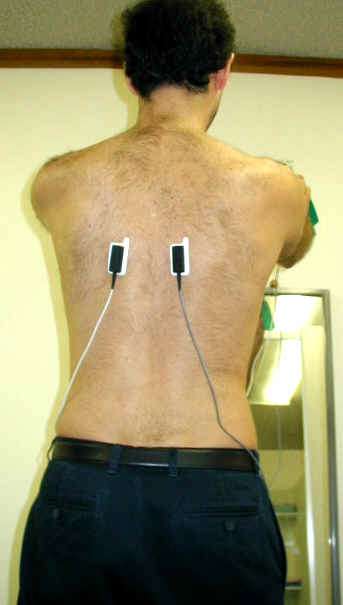
EMG biofeedback
Altered immune responses and altered lipid metabolism have been implicated as a causative factor in shoulder tendinopathies. Interested readers should look at Exercise and the Immune System as well as Exercise and Weight Loss elsewhere on this website for further explanations.
Sodium Hyaluronate and Platlet Rich Plasma (PRP) for partial thickness rotator cuff tears
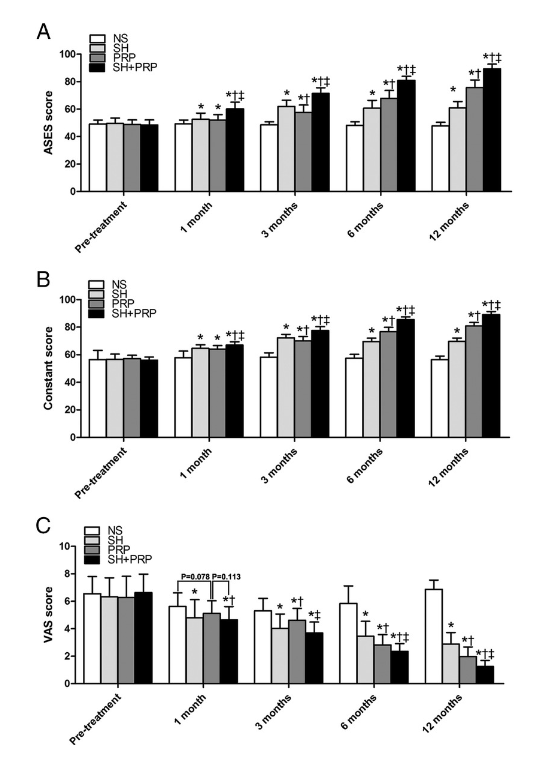
Investigations have demonstrated improvements in pain and function, in small to medium sized supraspinatus tendon tears, up to 12 months after PRP and Sodium Hyaluronate injections, in 45 people who received PRP injections and 48 people who had a combination of sodium hyaluronate and PRP injections (Cai et al 2019, Med sc Sp Ex, 51, 2, 227-233).
Interesting articles
these articles are particularly interesting in respect to synergistic 'timing' of muscle action in the upper and lower limbs
Commerford & Mottram (2001). Functional stability re-training: principles and strategies for managing mechanical dyfunction. Manual Therapy, 6,1, 3-14
Commerford & Mottram (2001). Movement and stability dysfunction - contemporary developments. Manual Therapy, 6,1, 15-26
Animated muscular synergistic interaction for shoulder abduction - refer to Climbing section
Shoulder Problems(English)
Schulter Probleme (Deutsch)
Last update : 4 November 2021