Carpal Tunnel Syndrome (CTS)
by Martin Krause
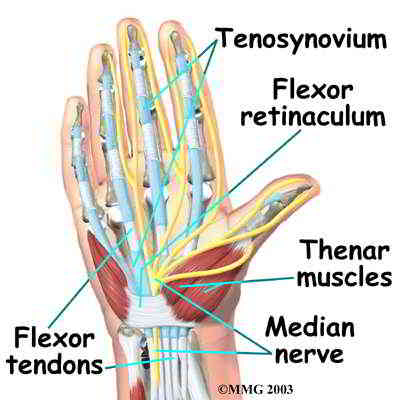
Carpal tunnel syndrome (CTS) is frequently described as a median nerve neuropathy caused by blood perfusion problems due to compression from tendon pathology at the wrist. Additionally, the brachial plexus has been implicated in muscle spasms (eg reduced upper limb tension testing range of motion) as well as 'double crush' injuries of the peripheral nerve. However, there may be a form of carpal tunnel symptomatology which involves the upper cervical spine and thoracic outlet syndrome (TOS). TOS has classically been attributed to compression of blood vessels of the anterolateral cervicothoracic triangle formed between the scalene muscles and the first rib. Scalene muscles are thought to become tight in upper chest breathers, in people with cervical ribs and as a compensatory mechanism for trapezius-serratus anterior dysfunction.
Symptoms of TOS have usually been described as pins & needles/numbness in the medial forearm (C8/T1 distribution). However, the upper cervical spine innervates the scalene and trapezius muscles as well as the diaphragm. Dysfunction of the upper cervical spine has the potential to result from overuse of the upper trapezius and levator scapula. This can lead to excessive compression of these joint causing neural irritation. Such irritation can create ectopic impulse generation into the spinal cord and scalene muscles whose tightness has been commonly implicated TOS. Due to the nature of TOS, muscles in the forearm can have their blood perfusion reduced, leading to premature fatigue and tightness. Importantly, the traditional examination procedures (Adson's manoeuvre, etc) for TOS aren't considered reliable unless taken into the context of the entire clinical reasoning process.
Scalene overuse may be a direct compensatory mechanism for reduced lateral excursion of the diaphragm in the inferior thorax. Additionally, this reduction in diaphragm function results in reduced core stability of the lumbar spine. Associated with reduced core stability are altered thoraco-lumbar fascia biomechanics with a potential increase in the tension of the latissimus dorsi. Increased tension of the latissimus dorsi affects scapula mobility at it's inferior angle, by reducing rib excursion, which may have a profound affect on serratus anterior function, as well as creating a 'tug-of-war' between the upper trapezius and latissimus dorsi.
Scapula mobility & stability are paramount considerations when treating a person who is suffering from TOS. Importantly, rehabilitation programmes should use exercises for eccentric and concentric strengthening of the serratus anterior and trapezius muscles. Additionally, stretches are incorporated for the scalene muscles and levator scapula, as well as soft tissue massage of these structures as well as pectoralis minor. Manual therapy techniques including joint mobilisations to the upper cervical spine, the cervico-thoracic junction, ribs and low thoracic spine, are combined with a home programme of Mulligan's NAG's, SNAG's and MWM's. In particular, self mobilisations of the upper ribs can be extremely useful in reducing scalene muscle tone as well as potentially afecting the ganglion stellatum. Taping of the inferior & superolateral angles of the scapula may enhance proprioceptive input, as well as 'unload' overused structures. Lateral diaphragmatic breathing and thoracic lateral flexion stretching is also important. Any excessive thoracic kyphosis will need to be addressed with joint mobilisation and appropriate exercise. Dry needling can be very useful in the treatment of overactive trigger points in the trapezius and levator scapula. However, care needs to be taken to avoid vital organs such as a pneumothorax if dry needling over lung fields. Naturally, any median nerve dysfunction in the remaining areas of the cervical spine should be addressed. Sympathetic nervous system function should also improve with enhanced thoracic spine mobility. Neural 'sliders' are also a useful part of a home exercise program.
Vascular Conditions
Virchow's Triad in the aetiology of thrombosis may be of assistence with differential diagnosis of vascular disease. The 3 variables include
- Changes in vessel wall (endothelial damage)
- Changes in blood flow (flow volume/stasis)
- Changes in blood constituents (state of coagulability)
The latter may include screening questions for blood disordes (thrombolytic ones, reactive protein C, as well as Thalasaemia and Sickle Cell Anaemia), systemic inflammatory conditions (such as Lupus and Scleroderma), the use of oral contraceptives, smoking, diet and frequent flying.
Taylor & Kerry (2005) quote a paper from Sise et al (1989) reporting an average 2 year delay in diagnosis in young people where 93% could have been diagnosed with simple palpation of peripheral pulses.
Familial history may be important in differential diagnosis of vascular conditions. Additionally, a history of heavy smoking can lead to internal blood vessel pathology. Similarly, women who take the pill may also be at risk. Aortic stenosis may manifest as a result of arterosclerosis or due to underlying congenital defects. These are screening questions which need to be asked during the subjective examination. During the physical examination, the radial and brachial pulses should be examined at rest but usually need to be assessed immediately after exercise or in the compromising posture where symptoms normally manifest. Further testing should include ankle blood pressure monitoring of each side. Taylor & Kerry (2005) recommend 20 minutes of rest before testing systolic blood pressure in the left and right brachial artery, posterior tibial and dorsalis pedis and then using the "Ankle to brachial pressure index = Ankle systolic BP / Brachial systolic BP". 1 - 1.2 considered normal, 0.75 - 0.9 indicates moderate disease, 0.5 - 0.75 severe disease and <0.5 is limb threatening (see: Taylor AJ, Kerry R, 2005, Vascular syndromes presenting as pain of spinal origin. Ch 36 in Grieve's Modern Manual Therapy: The Vertebral Column. Ed Boyling JD & Jull GA Elsevier Churchill Livingstone).
The posture and type of injuries associated with certain sporting pursuits such as cycling (and rowing) may make these athletes particularly prone to upper limb and head/neck vascular conditions. Additionally, one of the most common cycling injuries involves landing on the shoulder or outstretched hand resulting in possible neurovascular traction injury, direct trauma and/or clavicular fracture. The latter has been associated with trapezius muscle dysfunction which can be a precipitating variable leading to Thoracic Outlet Syndrome (TOS). Symptoms of TOS can include typical symptoms of neck, shoulder, elbow and hand pain. Occasionally, people describe a sense of swelling (or fullness) in the arm, with/without concommitant pins & needles or numbess. Vascular components of TOS may be less prevelant than neurological ones, yet this may be due to mis-diagnosis as the plethora of tests (Adson's, Allen's Halstead's manoeuver, Roos's EAST test) may be falsely positive or negative and variable b/n examiners. Hence, the examination must use the multitude of variables at the clinicians disposal, both Subjective symptoms & Physical signs - inductive and deductive reasoning, to make sense of the clincal picture. When in doubt and further investigations are required, by using the weight of probability from many variables, it may also make the argument for further testing more convincing to a medical colleague.
Paget - Schroetter syndrome is a deep venous thrombosis of the subclavian - axillary venous system, also known as "effort thrombosis" (Rutherford 1998, Zell et al 2001) and may account for about 3-7% of all DVT's (Taylor & Kerry 2005). The average patient is in their late 20's to early 30's and males present 3 times more commonly than females. Most commonly complain of quick insidious arm pain (70% in dominant arm), with possible supraclavicular fossa and ipsilateral neck pain. Most commonly occurs in activity with repetitve upper arm, over shoulder height, movements. The usual aetiology is Virchow's Triad which means that specific screening questioning is required. Additionally, other risk factors may include thoracic outlet factors such as cervical rib, anomalous first rib, hypertrophy of the anterior scalene, subclavius or pectoralis minor as well as endogenous factors such as activated protein C resistance and anticardiolipin antibodies (Ellis 2000 in Taylor & Kerry 2005).
Taylor & Kerry suggest that observable signs of vascular compromise may include skin pallor or cyanosis - both resting and positional, swelling, and/or superficial venous dilation. Corneal arcus or xanthelasmas (yellowish raises skin changes) around both eyes may be associated with hyperlipidaemia and hypercholesterolaemia. Staining of fingers may be a more accurate indicator of tobacco consumption. Obesity and state of mental awareness may also reflect underlying cerebrovascular state.
Hand and digital examination should also include nail squeezing - indicative of capillary refilling time. These should be perfomed in various positions of potential vascular compromise. Nail abnormalities may be present. Pulses should be tested, stethescope auscultation should be undertaken and the pressure cuff sphygmomanometer and hand held doppler or automatic blood pressure monitor used (Taylor & Kerry 2005).
Taylor & Kerry (2005) argue quite strongly that vascular examination is such a miniscule part of both under-graduate and post-graduate degrees that we may be implicated in delayed diagnosis as well as the initiating of innapropriate treatment.
Mind Map for CTS
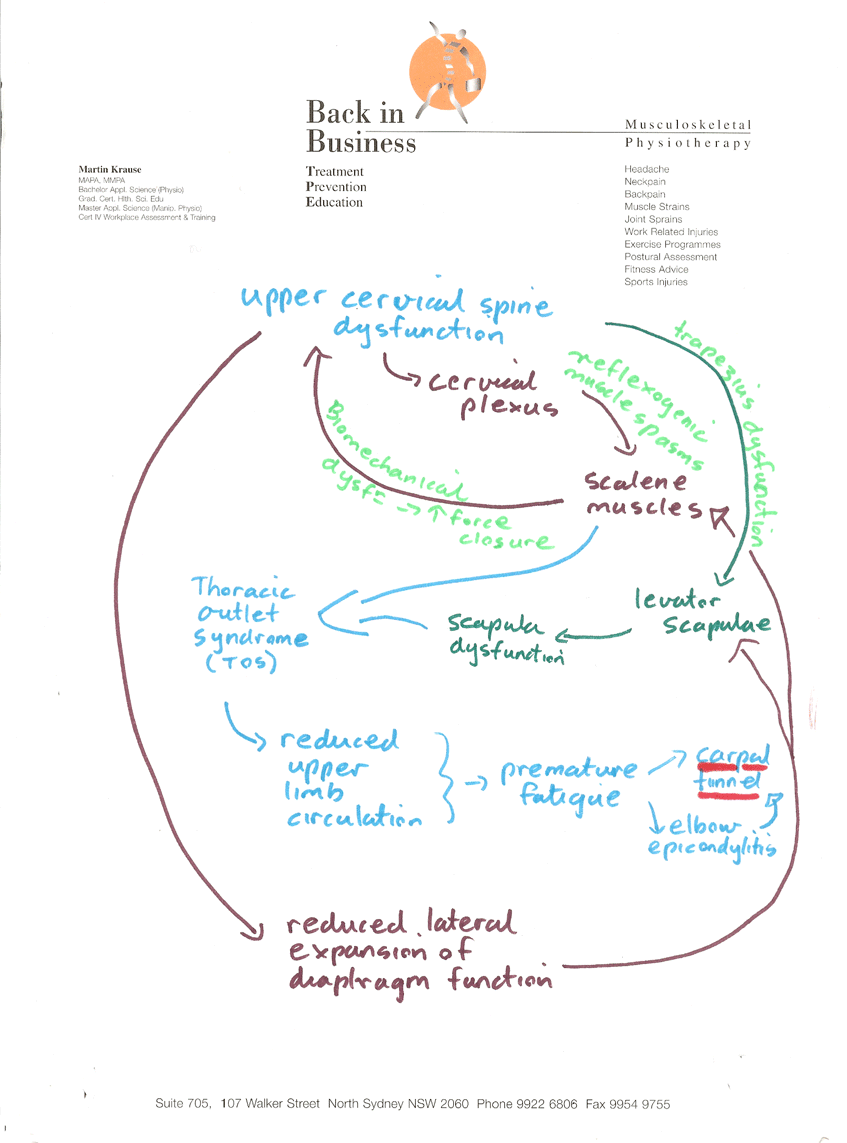
Importantly, examination and treatment of the scapulo-thoracic/cervical region along with examination of the carpal tunnel structures should be included at the initial consultation before the client goes rushing off to surgery. Although, many structures have been implicated in generating symptoms of carpal tunnel syndrome, the clinical reasoning process should clarify the extent of involvement of each and every structure. Confusion should be minimized through systematic assessment, treatment and exercise prioritization which reflect the clear explanations given to the client of predicted outcome.
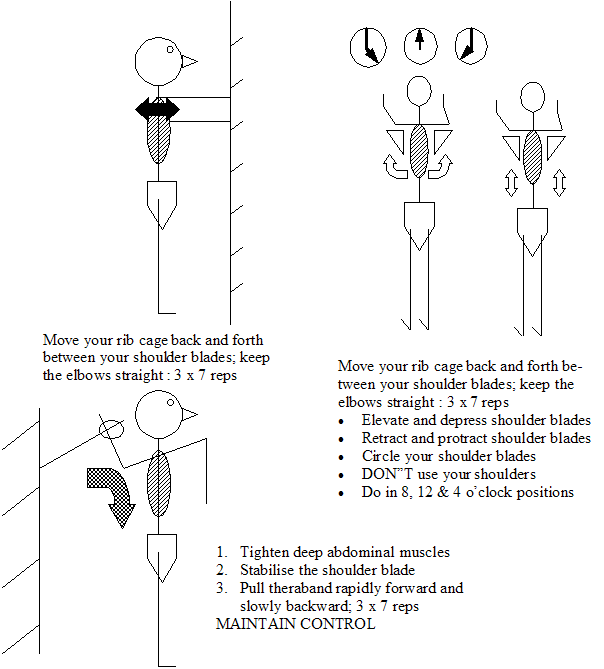
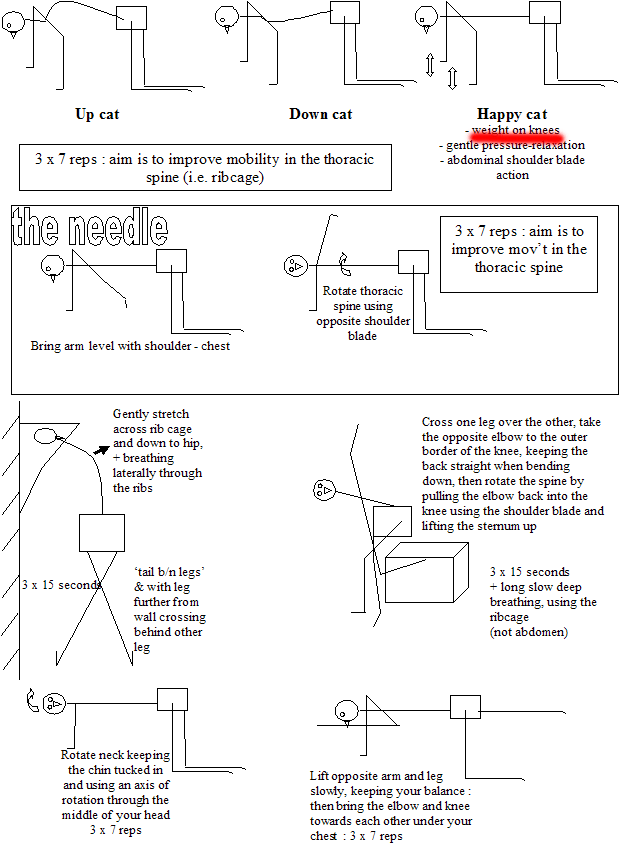
As symptoms improve and mild weight bearing can be tolerated then 4 point kneeling exercises using a yoga mat may be commenced
Last update : 6 January 2008

























































































































